Study hints at new approaches to prevent transplant rejection
To prevent the rejection of newly transplanted organs and cells, patients must take medicines that weaken their entire immune systems. Such potentially life-saving treatments can, paradoxically, leave those receiving them susceptible to life-threatening infections.
Now researchers at the University of North Carolina at Chapel Hill School of Medicine and the UNC Lineberger Comprehensive Cancer Center have discovered what seems to trigger the immune system to attack transplanted cells in the first place.
The finding could help chart a course to completely new therapies that may prevent graft-versus-host disease - the main cause of transplant failure - and its sometimes fatal complications.
The UNC study has identified a subset of cells - named TH17 cells - that can bring about the condition. Until now, without a clear understanding of the disease, clinicians have had little choice but to treat transplant patients with toxic regimens of steroids and immunosuppressive drugs.
"Our hope is that uncovering the mechanisms that cause graft-versus-host disease will allow for treatments that specifically target its causes and do not have the harmful side effects of traditional immunosuppressive therapy," said study lead author Jonathan S. Serody, M.D., a member of the Lineberger Center and the Elizabeth Thomas Professor of Medicine, Microbiology and Immunology at UNC. The results of the study appeared in the Feb. 5, 2009, issue of Blood, the journal of the American Society of Hematology.
Graft-versus-host disease (GVHD) is a serious complication of transplants that occurs when the donor's marrow (graft) produces immune cells that attack multiple organs of the recipient (host), typically the skin, gastrointestinal tract and liver.
Until recently, scientists believed that most of the disease's problems came from the production of specific molecules called interferons, a class of proteins that arise in response to foreign agents like viruses and parasites.
However, when several researchers tried testing whether or not blocking the action of these proteins would diminish graft-versus-host, they found that getting rid of interferons actually made the disease worse. When Serody and his colleagues tried this experiment themselves, they found that blocking the action of interferons resulted in a huge increase in the number of a specific group of white blood cells, or T lymphocytes, called TH17 cells.
To determine if these cells were actually aggravating the disease, the UNC researchers first cultured, expanded and purified cells of the TH17 lineage. In a technique pioneered by Michael J. Carlson, Ph.D., a postdoctoral fellow in Serody's laboratory, immature lymphocytes were incubated in petri dishes with a cocktail of proteins that "programmed" virtually all of them to become TH17 cells.
When the researchers transplanted the purified cells into mice, they found that the cells did in fact cause graft-versus-host disease, with the most severe damage to the lung and skin. Not only did these findings implicate TH17 cells in the disease, but they also generated one of the first mouse models to display acute GVHD skin changes - consistent with the most common manifestations of the disease in humans.
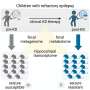
Having identified the role TH17 cells play in the disease, Serody and his colleagues then wanted to know what substances the cells were producing to cause it. They knew that TH17 cells produce a number of specialized proteins - called inflammatory cytokines - that are involved in communication between cells during the immune response. So they methodically blocked the action of each of these cytokines to determine which ones were actually causing the damage to various organs of the transplanted mice they were studying.
They found that the skin damage appeared to stem from the production of IL17 and its sister cytokines, while destruction in other tissues came from a protein called TNF-alpha. Interestingly, these findings lend support to the strategy employed by some clinicians to treat the manifestations of the disease with drugs that block TNF-alpha.
"For our findings to ever make an impact clinically, we would have to confirm that there are two main branches leading to the disease," said Serody. "Then we would need to take an approach that neutralizes both - simultaneously blocking the original suspect, interferon gamma, and our newest culprit, cytokines made by TH17 cells, to treat GVHD."
Research on that TH17 branch has already sparked the interest of some pharmaceutical companies such as Wyeth, and Serody predicts that there will be a number of drugs coming out in the next five years to treat immune-based skin diseases.
Source: University of North Carolina School of Medicine