The Hsp90-Antifungal Combo, please: Compromising fungi in the immunocompromised

Even the most drug-resistant fungi can be eradicated in multiple in vitro and in vivo models using a lethal combination of an antifungal agent and inhibition of the heat shock protein Hsp90, according to a new study by Whitehead Institute and University of Toronto researchers. The findings could enable development of novel antifungal therapies for patients with compromised immune systems.
Immunocompromised individuals--including HIV, chemotherapy, and organ transfer patients--with resistant fungal infections suffer mortality rates ranging from 50 to 90 percent.
"Being a pediatric oncologist, I have seen many unfortunate patients die from resistant fungal infections," says Luke Whitesell, a scientist in the lab of Whitehead Member Susan Lindquist. "It's incredibly frustrating to see a child with their cancer in remission being slowly eaten alive by a fungus like Aspergillus, and there's nothing you can do about it."
The development of effective antifungal drugs is limited by humans' close evolutionary relationship with fungi, and, in recent years, fungi's ever-evolving resistance to existing drugs. Former Lindquist postdoctoral researcher and lead author of this study, Leah Cowen, explains: "The drugs just don't wipe out the infection. So you wind up with a small population of fungi living in a host that is exposed to the drug for a long time, which favors evolution of drug resistance."
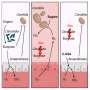
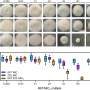
Previous studies suggested that Hsp90, which is found in both fungi and humans, plays a vital role in the evolution of drug resistance. In this most recent study, which appears in the February 24 issue of the Proceedings of the National Academy of Science (PNAS), Whitehead researchers tested Hsp90 inhibitors in combination with common antifungal drugs in an attempt to block the growth of Candida albicans and Aspergillus fumigatus, two of the most prevalent and lethal species that cause fungal infections in humans.
The researchers found that when antifungals or Hsp90 inhibitors are used individually, they are ineffective; however, when paired they form a deadly duo.
"When you combine the two, you reduce Hsp90 function enough that the fungi can no longer mount the crucial stress responses to antifungals required for survival," says Cowen. "So you cripple the fungus by severely compromising its stress responses."
According to Lindquist, "This is an entirely new strategy for making fungi susceptible to preexisting drugs and for preventing fungi from deploying the resistance mechanisms, which they have evolved against those compounds. It could make the difference between life and death."
Because Hsp90 is highly conserved, finding a compound to turn off Hsp90 in fungi, but not in humans, is a significant hurdle scientists must overcome. In addition, current Hsp90 inhibitors are toxic in mice with resistant fungal infections. To find promising Hsp90 inhibitors for antifungal therapy, Lindquist's lab has received a grant from the Molecular Libraries Probe Center Network (MLPCN) Program of the National Institutes of Health. The grant will allow researchers to screen large numbers of compounds in the search for potential fungus-selective Hsp90 inhibitors.
Still, even if the screen is successful, the battle between humans and fungi is not over.
"Eventually, like most drugs, Hsp90 inhibitors too, will become subject to resistance," suggests Lindquist, who is also a Howard Hughes Medical Institute investigator and professor of biology at MIT. "But in the meantime, these inhibitors will open a very large window of opportunity for individuals with resistant fungal infections."
More information: "Harnessing Hsp90 Function as a Powerful, Broadly Effective Therapeutic Strategy for Fungal Infectious Disease"
PNAS, February 24, 2009
Source: Whitehead Institute for Biomedical Research