Brain imaging may help diagnose autism
Children with autism spectrum disorders (ASDs) process sound and language a fraction of a second slower than children without ASDs, and measuring magnetic signals that mark this delay may become a standardized way to diagnose autism.
Researchers at The Children’s Hospital of Philadelphia report their findings in an online article in the journal Autism Research, published today.
“More work needs to be done before this can become a standard tool, but this pattern of delayed brain response may be refined into the first imaging biomarker for autism,” said study leader Timothy P.L. Roberts, Ph.D., vice chair of Radiology Research at Children’s Hospital.
ASDs are a group of childhood neurodevelopmental disorders that cause impairments in verbal communication, social interaction and behavior. ASDs are currently estimated to affect as many as one percent of U.S. children, according to a recent CDC report.
Like many neurodevelopmental disorders, in the absence of objective biological measurements, psychologists and other caregivers rely on clinical judgments such as observations of behavior to diagnose ASDs, often not until a child reaches school age. If researchers can develop imaging results into standardized diagnostic tests, they may be able to diagnose ASDs as early as infancy, permitting possible earlier intervention with treatments. They also may be able to differentiate types of ASDs (classic autism, Asperger’s syndrome or other types) in individual patients.
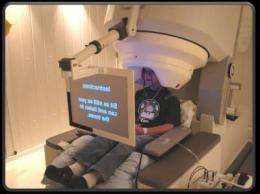
In the current study, Roberts and colleagues used magnetoencephalography (MEG), which detects magnetic fields in the brain, similar to the way electroencephalography (EEG) detects electrical fields. Using a helmet that surrounds the child’s head, the team presents a series of recorded beeps, vowels and sentences. As the child’s brain responds to each sound, noninvasive detectors in the MEG machine analyze the brain’s changing magnetic fields.
The researchers compared 25 children with ASDs, having a mean age of 10 years, to 17 age-matched typically developing children. The children with ASDs had an average delay of 11 milliseconds (about 1/100 of a second) in their brain responses to sounds, compared to the control children. Among the group with ASDs, the delays were similar, whether or not the children had language impairments.
“This delayed response suggests that the auditory system may be slower to develop and mature in children with ASDs,” said Roberts. An 11-millisecond delay is brief, but it means, for instance, that a child with ASD, on hearing the word ‘elephant’ is still processing the ‘el’ sound while other children have moved on. The delays may cascade as a conversation progresses, and the child may lag behind typically developing peers.”
A 2009 study by Roberts and colleagues sheds light on how changes in brain anatomy may account for the delays in sound processing. The study team used MEG to analyze the development of white matter in the brains of 26 typically developing children and adolescents. Because white matter carries electrical signals in the brain, signaling speed improves when neurons are better protected with an insulating sheath of a membrane material called myelin.
In this previous study, the researchers showed that normal age-related development of greater myelination corresponds with faster auditory responses in the brain. “The delayed auditory response that we find in children with ASDs may reflect delayed white matter development in these children,” said Roberts.
Roberts says his team’s further studies will seek to refine their imaging techniques to determine that their biomarker is specific to ASDs, and will investigate other MEG patterns found in children with ASDs in addition to auditory delays.















