Intestinal enzyme helps maintain population of beneficial bacteria
An enzyme that keeps intestinal bacteria out of the bloodstream may also play an important role in maintaining the normal microbial population of the gastrointestinal system. Since the loss of beneficial bacteria that usually results from antibiotic therapy can sometimes lead to serious health problems, a treatment that maintains microbial levels could have significant benefits.
"Our mouse studies confirmed that giving this enzyme by mouth keeps the gut healthy, in terms of the microbes that usually live there," says Richard Hodin, MD, of the Massachusetts General Hospital (MGH) Department of Surgery, senior author of the report in the November issue of the journal Gut. "This could prevent infection with dangerous bacteria like Salmonella and C. difficile, which can occur when the normal bacterial population becomes depleted, and may lead to development of a supplement to maintain intestinal health whenever someone takes an antibiotic."
Virtually all higher animals maintain a population of microbes – primarily bacteria – in their digestive tracts. These organisms are not only harmless, they also benefit their host by helping with digestion, and their presence prevents the more pathogenic bacteria that may be present from proliferating. Because antibiotics kill all non-resistant bacteria, including those residing in the intestines, the usual balance of beneficial versus harmful microbes is destroyed, leading to problems ranging from diarrhea to infections with dangerous antibiotic-resistant organisms.
A 2008 study by members of Hodin's team that investigated why intestinal bacteria and their toxins do not pass into the bloodstream found that intestinal alkaline phosphatase (IAP), an enzyme produced by the intestinal lining, blocks the activity of a toxic molecule found on many pathogenic bacteria. Because that study and findings by other groups showed that IAP acts against several bacterial toxins, the MGH researchers looked at whether the enzyme directly interacted with intestinal bacteria.
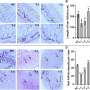
Studies of mice lacking the gene for IAP revealed that the animals had reduced levels of all intestinal bacteria and practically none of the common beneficial strains of E. coli. In fact, the most common E. coli strain would not grow if introduced into these knockout mice. But when the animals received oral doses of IAP, beneficial E. coli proliferated quickly after other microbial species were killed by antibiotics. Experiments with normal mice infected with an antibiotic-resistant Salmonella strain showed that IAP treatment significantly reduced Salmonella levels in the animals' feces. Although only 20 percent of animals not treated with IAP survived, 70 percent of those receiving the enzyme were alive 7 days later.
"We believe that IAP rapidly restores E. coli and other beneficial bacteria after antibiotic treatment and that the higher numbers of these bacteria prevent colonization by Salmonella or other pathogens by competing for nutrients and attachment sites," says Mahdu Malo, PhD, MBBS, of MGH Surgery, corresponding and first author of the Gut paper. "We need to test this approach in larger animals before planning a human clinical trial, but this approach has the potential of solving a common, often serious health problem."