Improving life for those who suffer most from type 1 diabetes

A transplant procedure given only to those with Type 1 diabetes who pass out repeatedly from low blood sugar levels, or ‘hypos’, is likely to become much more effective as a result of a discovery made by a group of Australian researchers.
‘Islet transplants’ (the transplant of islets from the pancreas, which contain insulin-producing cells) are not given lightly because recipients must take immunosuppressive drugs for the rest of their lives. As a result, transplant recipients are generally people who cannot regulate their blood sugar levels, and who lapse into comas, often without warning.
However, many islets die within a week of transplantation, and most patients have to go back on at least some insulin within 2-5 years.
Associate Professor Jenny Gunton, from Sydney’s Garvan Institute of Medical Research and Westmead Hospital, together with the Westmead Islet Transplant Program, has discovered that treating islets prior to transplantation with a drug that boosts production of the HIF-1 alpha protein (a master regulator of cell survival) significantly improves the survival of human islets in mouse recipients. Her findings are published in Cell Transplantation, now online.
“I work with the islet transplant team at Westmead Hospital, and we’ve been trying to figure out a way of improving outcomes for people who receive islet transplants,” she said.
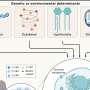
“Isolating islets from a donor pancreas exposes them to lack of oxygen, and islets suffer a lot of damage even from temporary low amounts of oxygen. HIF-1 alpha helps cells respond to low oxygen levels, and so we predicted that boosting it would improve islet survival.”
“When we tested the effect of treating islets prior to transplantation with the drug deferoxamine, DFO for short, which boosts HIF-1 alpha, the results supported our prediction.
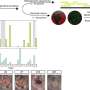
“Because we had to test the effect before using it in people, we transplanted human islets into mice – with some islets having been treated with DFO, and some not treated. In a ‘minimal mass’ model, which approximates the human situation, we went from a 0% cure rate at a month to a 50% cure rate in a month.”
“In an ‘adequate mass’ model, where you give the mice many more islets, mice were cured by non-DFO-treated islets. However, it took over 3 times the number of non-DFO-treated islets to cure the mice.”
“We also conducted an experiment which demonstrated the importance of HIF-1 alpha – by engineering mice not to produce any HIF-1 alpha in their insulin-producing cells. When these non-HIFF-1 alpha islets were transplanted into diabetic mice, the recipients did very badly.”
“The good thing about deferoxamine is that it is already approved for human use, has been in use for well over a decade, and in our studies, we used it the normal human treatment dose.”
“At Westmead, we’ve already started using DFO to treat islets before transplantation. While it’s still too early to draw any conclusions, recipients are doing well. To actually test the effect in people properly, you’d need to do a big randomized, placebo-controlled trial, and to get the number of people needed you’d have to enrol patients from many centres world-wide – clearly not an easy option.”
“We hope that finding a way of improving islet survival in recipients will extend the usefulness of donor pancreases – meaning you could give more transplants because one pancreas might be enough for one recipient, instead of two to three pancreases for each recipient.”
“At the moment islet transplants are good for those people that have regular severe hypos. Even if the transplanted islets don’t get the person ‘off’ insulin, they stop experiencing hypos. This increases quality of life immeasurably because prior to transplantation repeat hypo sufferers are not allowed to drive and generally can’t hold down a job.”
“We hope our finding will give these people a longer window without insulin use.”










.jpg)