Abnormal involuntary eye movements in amblyopia linked to changes in subcortical regions of brain
Little is known about oculomotor function in amblyopia, or "lazy eye," despite the special role of eye movements in vision. A group of scientists has discovered that abnormal visual processing and circuitry in the brain have an impact on fixational saccades (FSs), involuntary eye movements that occur during fixation and are important for the maintenance of vision. The results, which raise the question of whether the alterations in FS are the cause or the effect of amblyopia and have implications for amblyopia treatment, are available online in advance of publication in the November issue of Restorative Neurology and Neuroscience.
"Although FSs are of great functional significance in neural coding, visual perception, and visual task execution, their behavioral characteristics in visual and neurological disease have been rarely studied," says lead investigator Xue-Feng F. Shi, MD, PhD, of the Tianjin Key Laboratory of Ophthalmology and Visual Science, Tianjin Eye Institute, College of Clinical Ophthalmology, Tianjin Medical University, and the Department of Pediatric Ophthalmology and Strabismus, Tianjin Eye Hospital, Tianjin, China. "We carried out quantitative and detailed analysis of fixational saccades in amblyopia for the first time."
Investigators examined 28 patients with amblyopia and 28 age-matched control subjects. Using a high-speed eye-tracker, fixational eye movements of both eyes were recorded. A computerized analysis of eye-movement waveforms was developed to quantify the parameters of FSs, and a simulation model was used to explore the neural mechanism of changes in fixational saccadic performance of amblyopic eyes.
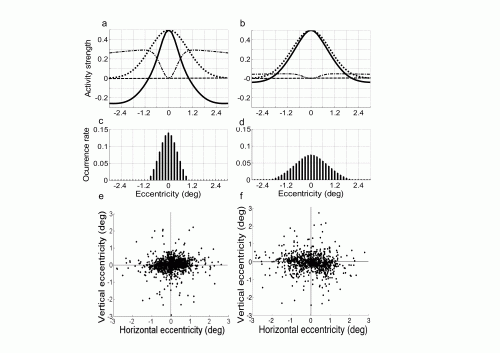
Amblyopic eyes showed fewer FSs than control eyes, but they had increased amplitudes and speed. Periods between movements were significantly longer in amblyopic eyes. FS was suppressed mainly for those with amplitudes smaller than 0.6 degrees, but was increased for those greater than 0.6 degrees. "We conclude that the change of amplitude distribution is a dominant alteration of FSs in amblyopia, while the change of other parameters is secondary. These findings should provide the necessary baseline information for future studies and should advance our understanding of the correlation between visual system impairment and eye-movement behavior," notes Dr. Shi. The simulation model suggests that an excitatory-inhibitory activity imbalance in the superior colliculus (SC) of the brain, an area involved with vision and eye movement, may explain these changes.
Dr. Shi explains that there are two possible interpretations of the study. "Altered FSs may be an effect of amblyopia, an attempt of the visual system to try to capture more information from a broader spatial domain to enhance contrast sensitivity, which is reduced in lazy eye. Or it may be the cause or a contributing factor to the original deficit, which may open up a new avenue for the research of the neural mechanisms of amblyopia that will be as different from the traditional research route as the pioneering work in visual cortex by Hubel and Wiesel (Nobel Laureates). Another issue of particular interest is whether amblyopia treatment and visual training can positively influence FS," he says. "To solve these questions will be a major step forward in our understanding of visual system and eye movement impairments which then provides a new starting point for innovative therapeutic approaches."
More information: "Fixational Saccadic Eye Movements are Altered in Anisometropic Amblyopia," by Xue-feng F. Shi, Li-Min Xu, Yao Li, Ting Wang, Kan-xing Zhao, and Bernhard A. Sabel. Restorative Neurology and Neuroscience, 30:6 (November 2012). DOI: 10.3233/RNN-2012-129000













