Novel one-step system for restoring voice in throat cancer patients
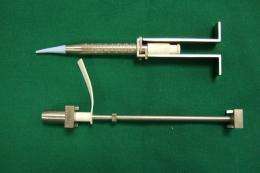
Patients who have lost their voice box through disease such as throat cancer may be able to speak immediately after a procedure to create a small opening at the throat. A novel system developed through an Engineering-in-Medicine project led by Dr Chui Chee Kiong, NUS Department of Mechanical Engineering, and Dr David Lau, Consultant Ear, Nose & Throat (ENT) Surgeon at Raffles Hospital, cuts down a two-week duration before patients can speak, to about 10 minutes after the initial procedure.
People who undergo laryngectomy and lose their voice box can recover approximately 80 per cent of normal speech by having a voice prosthesis fitted into an opening or fistula between the trachea (windpipe) and esophagus (food pipe). To speak, the patient covers the stoma (breathing opening in the neck) with his or her thumb and forces air through the prosthesis into the esophagus and out through the mouth. Before the prosthesis can be inserted, the doctor needs to make a small puncture (tracheo-esophageal puncture or TEP) in the wall between the trachea and esophagus. During the puncture, a guide-wire is inserted into the fistula to prevent the creation of false passages. Two "dilators" are inserted to widen the fistula, with the second one a little wider in circumference. Previously, a temporary rubber tube is placed into the fistula and the voice prosthesis is not inserted until about two weeks later, when the fistula is "mature". However, the new device changes this.
Explaining their invention, Dr Chui said, "We have merged all the steps into a single procedure. Most significantly, although doctors still need the nasal endoscope to guide and monitor progress during the procedure, our system ensures an immediate snug fit of the prosthesis in the passageway created between the trachea and the esophagus. Until now, this can take some trial and error to achieve good sizing of the prosthesis."
Voice prostheses vary in length for different individuals, depending on the thickness between the food pipe and the windpipe. The length of the TEP needs to be accurate. Usually, the length ranges between 6mm to 26mm. It is important that the prosthesis fits well otherwise it may be ineffective, or leak and cause discomfort.
Said Mr Chng Chin Boon, Research Engineer from NUS Department of Mechanical Engineering and member of the research team, "We added markings onto the cannula used for inserting the prosthesis. From the endoscopy, we would know the distance between the anterior esophageal wall (front wall of the food pipe) and the posterior tracheal wall (back wall of the windpipe), allowing us to size the prosthesis appropriately."
This takes away a lot of discomfort such as coughing and gagging, should the prosthesis need to be removed and fitted again if the measurement is not right.
"Most prostheses need to be changed due to wear and tear, depending on each individual. And each time, the size of the prosthesis to be inserted may differ due to tissue changes in the patient. Our invention will offer patients a more fuss-free system, cutting down time and discomfort. It will also cut down the cost for the patient as the number of procedures is reduced," added Mr Chng.
The system has been successfully tested on animals, and is now ready for clinical human trial.
Said Dr David Lau, "Patients requiring voice restoration after surgery for laryngeal cancer have to make multiple visits to the clinic, and I had often thought how a simple, one step solution would save them time, discomfort and money. So we decided to go out and design that solution."
Dr Lau added, "The system we designed has several advantages over existing methods as it not only reduces the number of steps and complexity, but also increases accuracy of placement and safety, and allows for immediate voicing. However patients will still need to put in some effort, and work with the speech therapist to get the best voicing results."


















