Use of antipsychotic drugs improves life expectancy for individuals with schizophrenia
Results of a Johns Hopkins study suggest that individuals with schizophrenia are significantly more likely to live longer if they take their antipsychotic drugs on schedule, avoid extremely high doses and also regularly see a mental health professional.
Psychiatrists have long known that people with schizophrenia who stick to a drug regimen have fewer of the debilitating delusions and hallucinations that are hallmarks of this illness. But there have been concerns about whether some of the known side effects of the medications—increased risk of cardiovascular disease and diabetes, for example—carry higher mortality risks, the researchers say.
"We know that antipsychotic medications reduce symptoms, and our study shows that staying on reasonable, recommended doses is associated with longer life," says Bernadette A. Cullen, M.B., B.Ch., B.A.O., MRCPsych, an assistant professor of psychiatry and behavioral sciences at the Johns Hopkins University School of Medicine, and leader of the study published in Schizophrenia Bulletin. "The same is true for going to see a psychiatrist or therapist," she says, noting that regular visits to a mental health professional are one way to monitor and encourage drug-use compliance, but also in and of themselves increased survival in this vulnerable population.
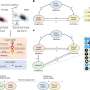
Cullen and her colleagues analyzed data collected between 1994 through 2004 on 2,132 adult Maryland Medicaid beneficiaries with schizophrenia. The researchers reviewed how much medication the patients took, how regularly they took it and how often they visited a mental health professional. The goal of the study was to review how adherence to the 2009 pharmacological Schizophrenia Patient Outcomes Research Team (PORT) guidelines was associated with mortality in this population.
Comparing data from year to year, the researchers found that among those patients who had 90 percent or better compliance with their medication schedules, the risk of death was 25 percent lower compared to those who were less than 10 percent compliant. Over the decade-long study period, taking medication did not increase the risk of death and there was a trend towards reducing the mortality rate. In addition, the researchers found that each additional visit per year to a mental health professional was linked to a 5 percent reduction in risk of death overall.
Cullen's study did not rule out all links between increased mortality and antipsychotic drugs. For example, her team found that people who took high doses of first-generation antipsychotic medication daily (1500 mg or greater chlorpromazine equivalents) were 88 percent more likely to die. She says mortality rates possibly increased in this group because first-generation antipsychotics have been associated with cardiac disease risks, and among those who died while taking the larger doses, 53 percent died of cardiovascular disease. "These drugs work very well, but there is clearly a point of diminishing returns," she says. "You rarely need to be on extremely high doses."
Among those whose information was reviewed, the most common cause of death was cardiovascular disease (28 percent); unintended harm, including suicide, was responsible for 8 percent.
"If people are taking their medications, they usually have fewer symptoms and are able to be more organized in other areas of their lives," says Cullen, director of community psychiatry at The Johns Hopkins Hospital. "We believe they are then more likely to make appointments with their primary care doctors, to stay on top of other illnesses they may have and to regularly take diabetes, blood pressure or cholesterol medication that they may require to stay healthy. We also believe that they are more likely to be socially engaged and have a healthier lifestyle."
"If your illness is under control, you can do a lot more," she adds.
Cullen says the study clearly lays out the value of mental health providers to individuals with schizophrenia. Those who saw therapists or psychiatrists were more likely to survive, regardless of whether the individual also took his or her antipsychotic medication on a regular basis, she says.
This finding is crucial, she says, given that Maryland Medicaid officials are considering capping the number of mental health visits allowed each year, something the data now suggest is potentially detrimental to survival.
Cullen notes that adherence to a medication regimen and moderate first-generation antipsychotic dosing are both part of the 2009 PORT recommendations designed to guide treatment.