Need to learn from incidents and near misses in the health care chain
Approximately 1,735 patients a year on average die in the Netherlands as a result of mistakes. Health care professionals try to learn from these incidents and near misses, but the learning process is often confined within the individual organizations and the individual links in the health care chain. But incidents and near misses occur just as much when patients are referred from one link to another. Research into communication between the various links on incidents and near misses shows up the weak spots in the learning process within the chain. On 9 November 2012 Greet van der Kaap, research lecturer at Windesheim University of Applied Sciences in Zwolle, is to receive her PhD from the University of Twente on 'The Weakest Link, inter-organisational communication about (near) incidents in the health care chain'.
Patients and professionals in the health service depend on the correct transfer of medical information from one link to another. If the information on a patient's medical condition is incorrect, an ambulance paramedic cannot provide the right care on the way to hospital. Or if a patient is allergic, everyone in the chain needs to know this. Something can go wrong in a link and only be discovered later on. Health care professionals can learn from these incidents and near misses by communicating about them.
Apples and oranges
But does every part of the chain speak the same language? Greet van der Kaap's study shows that different professions define incidents and near misses differently. Pharmacists and nurses often give specific examples, such as the wrong medication or mix-ups with names. For physicians and specialists this is much more of a grey area, concerning whether diagnoses are missed. In effect this is like comparing apples and oranges, and it hampers the learning process between the various links.
Problem-solving ability
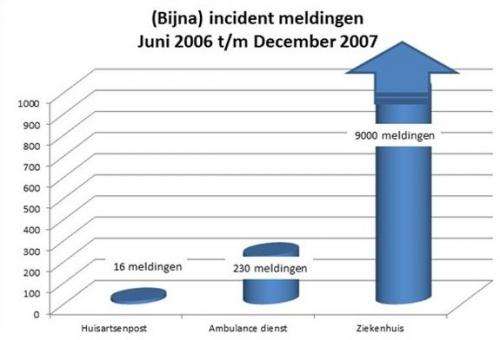
According to Van der Kaap, the combination of a high degree of problem-solving ability and a high degree of autonomy hampers communication on incidents and near misses, as can be seen for example in the case of GPs, specialists and nursing home doctors. The problem is solved: it's gone, so why talk about it? Professionals with a lower degree of autonomy, such as pharmacists and nurses, are more likely to communicate with other professions, as they are not allowed to take decisions on medicines themselves, they cannot prescribe a solution if something goes wrong. For the sake of inter-organizational learning, however, it is important for all professionals to communicate about incidents and near misses.
Solutions
Van der Kaap puts forward some solutions to improve learning within the health care chain. This will require a good balance between differentiation and integration. Professionals need to realize that they form part of a health care chain, and communication with one another on incidents and near misses is vital. Providing feedback to professionals in other links is inextricably linked with inter-organizational learning. A reporting system covering the entire chain, for example with certain weeks scheduled for reporting (putting everyone on alert every so often) could also help – provided it is organized in such a way that it does not involve a lot of red tape or place excessive demands on scarce resources such as time and money.