Doctors orders: A veteran of war and vascular surgery offers advice on health reform
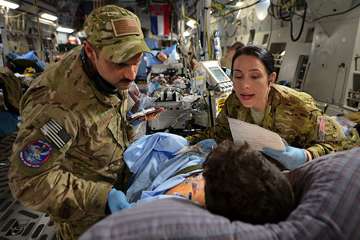
A weary American soldier rests on one knee in a dusty foreign desert. The young man's massive backpack is overflowing with equipment and there are pouches strapped to his belt, tools attached to his boots, and gear affixed to his helmet.
"He's straining under the load that the country has asked him to carry," said Jonathan Woodson, Assistant Secretary of Defense for Health Affairs, describing a photograph he shared at the Harvard Medical School Office of Diversity and Community Inclusion's 2013-2014 Leadership Forum on Oct. 28.
After more than 12 unbroken years of combat operations, the longest sustained period of war in American history, the American soldier has a right to be weary, Woodson said, explaining that his own job in the U.S. Defense Department has been to oversee the health care provided to the nation's military personnel.
"That's who we serve," Woodson said.
Woodson's presentation focused on the relationship between the U.S. armed forces and civil society, the contributions made by both academic and military practitioners that have benefited both groups, and the shared responsibility that military and civilian physicians and researchers have serving both soldiers and citizens.
Woodson, who trained as a vascular surgeon at Massachusetts General Hospital, was deployed as a medical officer in Saudi Arabia, Kosovo and Iraq. He also served as associate dean for diversity and multicultural affairs and professor of surgery at the Boston University School of Medicine while acting as senior attending vascular surgeon at Boston Medical Center. Woodson drew on his experience and insights from both of those worlds, outlining the opportunities and challenges that both worlds share.
In his current posting, Woodson said, he is responsible for the nation's military health enterprise, which includes force readiness, biomedical research, and the health insurance system for families of military personnel. The annual budget for this work is $53 billion.
Historically, Woodson said, military medicine has made significant contributions to the advancement of treatments for traumatic injury, shock and sepsis, and to the technology of surgery and medical evacuation.
Today, he said, the integrated defense health agency—with innovative, shared electronic medical records, patient-centered medical records, and comprehensive health education and population medicine approaches that are aimed at increasing individual engagement and participation in the production of their own health—also offers important insights into how the U.S. can improve health care for all its citizens.
For example, Woodson noted that the U.S. employs standards-based educational methods to train front-line military medics who sometimes have only high school educations. These medics go on to perform complex, life-saving battlefield medical procedures and, he said, the same training methods could be used to prepare a new corps of civilian medics to provide similar crucial primary care services in civilian communities.
As the nation develops new systems to meet the military and domestic health care needs of the future, Woodson said, it needs to develop an integrated system that effectively takes information, generates usable knowledge and then creates wisdom within the U.S. health care system.
"Wisdom is when we have everybody operating from an evidence-based strategy to the highest standards," Woodson said.