Study reveals how variant forms of APOE protein impact risk of Alzheimer's disease
Carrying a particular version of the gene for apolipoprotein E (APOE) is the major known genetic risk factor for the sporadic, late-onset form of Alzheimer's disease, but exactly how that variant confers increased risk has been controversial among researchers. Now an animal study led by Massachusetts General Hospital (MGH) investigators shows that even low levels of the Alzheimer's-associated APOE4 protein can increase the number and density of amyloid beta (A-beta) brain plaques, characteristic neuronal damage, and the amount of toxic soluble A-beta within the brain in mouse models of the disease. Introducing APOE2, a rare variant that has been associated with protection from developing Alzheimer's disease, into the brains of animals with established plaques actually reduced A-beta deposition, retention and neurotoxicity, suggesting the potential for gene-therapy-based treatment.
"Using a technique developed by our collaborators at the University of Iowa, we were able to get long-term expression of these human gene variants in the fluid that bathes the entire brain," says Bradley Hyman, MD, PhD, of the MassGeneral Institute for Neurodegenerative Disease (MGH-MIND), senior author of the report in the Nov. 20 Science Translational Medicine. "Our results suggest that strategies aimed at decreasing levels of APOE4, the harmful form of the protein, and increasing concentrations of protective variant APOE2 could be helpful to patients."
The association between the APOE4 variant and increased Alzheimer's risk was first made more than 20 years ago. Subsequent research has established that carrying two copies of the harmful variant increases risk 12 times compared with having two copies of the more common form, APOE3. Inheriting the APOE2 variant, however, appears to cut the risk in half. The extremely rare gene variants that directly cause the familial forms of the disease all participate in the production and deposition of A-beta, but exactly how APOE variants contribute to the process has been poorly understood.
Secreted by certain brain cells, APOE is known to regulate cholesterol metabolism within the brain and can bind to A-beta peptides, suggesting that the different forms of the protein may affect whether and how toxic A-beta plaques form. While previous investigations into the protein's effects have used either mice in which gene expression was knocked out or transgenic animals that expressed human gene variants throughout their lifetimes, the MGH-MIND-led study used a different approach to investigate the effects of introducing the variant forms of the protein into brains in which plaque formation had already begun. They directly injected into the cerebrospinal fluid of a mouse model of Alzheimer's – adult animals in which plaques were well established – viral vectors carrying genes for one of the three APOE variants or a control protein.
Two month after the vectors had been injected, about 10 percent of the APOE in the brains of animals that received one of the variants was found to be the introduced human version. At five months after injection, examination of brain tissue revealed that the A-beta plaques in mice that received APOE4 injections were more numerous and significantly denser than those of mice receiving APOE2. The growth of plaques in animals receiving APOE3 was intermediate between that of the other two groups and similar to what was seen in control animals. Levels of A-beta in the blood of mice that received APOE2 were higher than in the other groups, suggesting that the protective variant had increased clearance of A-beta from the brain.
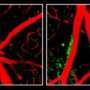
In a group of animals in which tiny implanted windows allowed direct imaging of brain tissue, the progression of A-beta plaque deposition was fastest in animals receiving APOE4 and slowest, sometimes even appearing to regress, in mice injected with APOE2. Signs of neuronal damage around plaques also varied depending on the APOE variant the animals received, and experiments in a different Alzheimer's model in which plaques appear more slowly showed that injection of APOE4 increased levels of free, soluble A-beta in the fluid that bathes the brain.
"This study has allowed us to sort out, in mice, which effects of the different types of APOE were most important to variation in amyloid plaque deposition," says Eloise Hudry, PhD, of MGH-MIND, lead author of the Science Translational Medicine report. "Our results imply that APOE-based therapeutic approaches may help to alleviate the progression of Alzheimer's disease. More study is needed to pursue that possibility and to investigate the potential use of this gene transfer technology to introduce other protective proteins into the brain."
More information: "Gene Transfer of Human Apoe Isoforms Results in Differential Modulation of Amyloid Deposition and Neurotoxicity in Mouse Brain," by E. Hudry et al. Science Translational Medicine, 2013.