Researchers explain why some wound infections become chronic
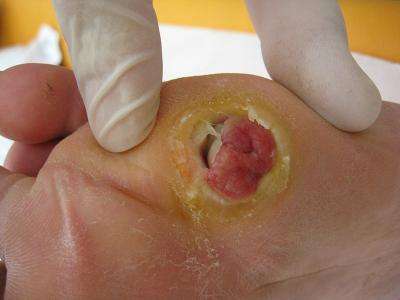
Chronic wounds affect an estimated 6.5 million Americans at an annual cost of about $25 billion. Further, foot blisters and other diabetic ulcers or sores account for the vast majority of foot and leg amputations in the United States today.
Why does treating chronic wounds cost so much? What complicates chronic wound infections, making healing difficult?
Manuela Martins-Green, a professor of cell biology at the University of California, Riverside, reports that two biological activities are out of control in chronic wound infections. These are reactive oxygen species (ROS), which are chemically reactive molecules formed by the partial reduction of oxygen, and biofilms that are formed by selective invading bacteria.
ROS is the natural byproduct of the normal oxygen metabolism and plays a role in cell signaling and homeostasis. However, excessive ROS can induce chronic inflammation, a key characteristic of wounds that do not heal. The biofilms are bacterial defense mechanisms. Together they create a toxic environment that can resist efforts to heal and close a chronic wound.
"By decreasing ROS levels within a chronic wound in a diabetic mouse model, my lab was able to normalize conditions and heal the wound," Martins-Green said. "Indeed, we saw significant improvement in healing the wound."
She announced her findings on Dec. 17 in New Orleans, La., at the 53rd annual meeting of the American Society for Cell Biology.
To identify the central role of ROS in maintaining chronic wound infection, Martins-Green's lab inhibited two antioxidant enzymes, glutathione peroxidase and catalase. Ordinarily, these enzymes help maintain normal tissue levels of ROS. But when they were inhibited, the amount of ROS in the wounds soared and the biofilm strengthened. The scientists also found that the two antioxidant enzymes were more damaging if they were inhibited in combination rather than individually.
Next, to decrease ROS to normal levels, the researchers applied two strong antioxidant supplements, vitamin E and N-Acetyl cysteine. As a result, the activities of the antioxidant enzymes glutathione peroxidase and catalase were restored, ROS levels decreased, and the bacterial biofilm disintegrated in the wound—all of which resulted in the development of healthier wound tissue and led to wound healing.
"Our results show for the first time that by deliberately modulating specific parameters, we can create chronic wounds and then reverse chronicity by antioxidant treatment," Martins-Green said. "These findings should help in unraveling the mechanisms underlying the development of chronic wounds and hence in identifying potential targets for treatment of these wounds in humans."
More information: Author will present, "Creating and reversing diabetic chronic wounds by manipulation of redox parameters," on Tuesday, Dec. 17, during the 12 noon to 1:30 p.m., poster session, "Defining Therapeutic Targets and New Therapeutics."














