California doctors work to speed up trauma care (Update)

Before the car-wreck victim reached the emergency room, doctors, residents and nurses at Cedars-Sinai Medical Center knew what to expect by glancing at their smartphones.
The details came in the staccato of text messages: A 35-year-old man had driven head-on into a bus. He suffered major chest injuries. His vital signs were crashing.
This was not just another day in the hospital. It was a laboratory billed as the "O.R. of the future," an ongoing experiment aimed at breaking down barriers that bog down care through open communication, better use of technology and teamwork.
In reality, trauma care is rarely this organized. But those who are prized for individual skills are increasingly learning that when it comes to treating trauma patients from accidents, natural disasters or terrorist bombings, communication and coordination can determine whether someone lives or dies.
At an office building less than a mile (1.6 kilometers) from the main Cedars-Sinai campus, doctors are experiment objects in simulations designed to test such skills.
There's a "mission control" room filled with video screens where trainers keep track of the action. The walls are see-through. Open workspaces are favored over cubicles.
At the heart of the lab is a room that could be outfitted as the ER, operating room or intensive care unit—depending on the practice of the day. Medical simulation labs have evolved over the years, from simple lifelike models of body parts that doctors train on to full-blown replications of hospital rooms where trainees can practice different situations. The Cedars-Sinai space strives to speed up trauma care by eliminating workflow disruptions and honing communication skills.
"Health care today is delivered more by teams rather than by individuals. We have to educate folks in teamwork skills," said William McGaghie, who heads a professional training institute at Loyola University Chicago Health Sciences Division.
Registered nurse Anna Doyle is used to working with doctors who parachute into the latest crisis, whether it's tending to the victim of a gunshot wound or rollover accident. It's often a chaotic scene, and not everyone takes the time to get to know one another.
During a recent rehearsal, a resident piped up and asked for everyone's names. For a second, it felt like the first day of school as introductions were made.
Doyle said she found the introductions calming—even if it was just practice.
"We had a personal moment ... that never happens," said Doyle, acknowledging that there's always a line of walking wounded in an emergency.
Armed with a $4 million grant from the Defense Department, doctors and nurses at Cedars-Sinai have been testing ways to improve trauma care by running simulations at the newly opened lab that has the feel of a tech startup.

"This is a place for experimentation," surgeon-in-chief Dr. Bruce Gewertz said.
Before the lab opened, Gewertz and his colleagues followed real trauma patients from the moment they were unloaded from the ambulance to their transfer to the ICU. Along the way, the team documented obstacles that slowed down care: Too many people spoke at the same time, prompting a nurse to ask a resident to speak up. A patient went for a CT scan only to find another patient already in the scanner. A resident's cellphone rang while scrubbing in.
Most of the time, researchers found, delays in care were caused by a lack of communication and logistical hurdles.
The goal is to get everyone on the same page during the "golden hour," a concept borrowed from military medicine when time is of the essence.
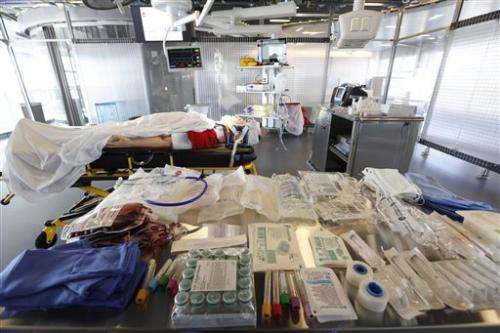
The team recently partnered with a consulting firm to develop an in-house iPhone app that displays a patient's vitals and blasts out the information to the trauma team as members are assembling. There's also a text-messaging feature that allows doctors and nurses swarming in from various parts of the hospital to communicate with one another before the patient arrives.
It's too early to determine how much it would cost if the app was part of routine care, but Gewertz said it'll be relatively inexpensive, involving the cost of the phones and a monthly license fee for protected data storage.
On a recent weekday, the team's cellphones buzzed with the condition of the first "patient" of the day, the bus-crash victim.
Typically, doctors don't know vitals until a nurse scrawls them on a whiteboard.
Apps can be helpful, allowing medical teams to "know the information en route so they're not coming in cold," said Pam Jeffries, president of the Society for Simulation in Healthcare and a professor at the Johns Hopkins University School of Nursing. Jeffries is not involved in the Cedars-Sinai effort.
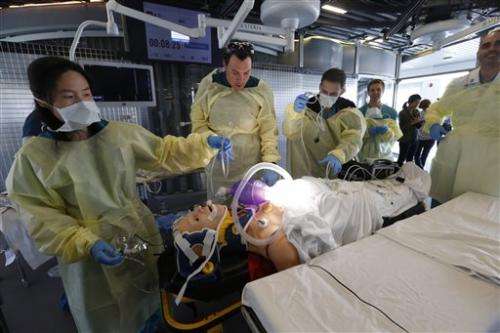
The patient—a high-tech dummy—was wheeled in, moaning and complaining. Doctors and nurses sprang into action, ripping off the dummy's clothes and placing a breathing tube before transferring him.
Despite the quick response, there were hiccups, mainly because of a lack of experience. Residents had trouble inserting the tube, and it took several tries to get it right.
For the second scenario, the team was not given advance information about the patient and kept going in circles asking for any details. A doctor said he heard it was a case of a pedestrian hit by a car.
"Do we know if it's male or female?" another asked.
"I don't know much more than auto versus" pedestrian, the doctor said.

The chief resident said there's worry about internal injuries and to make sure blood supply and other essentials were ready.
As if that weren't enough, they also had to deal with a fire—simulated smoke from dry ice was pumped into the room. One called out for the fire alarm to be shut off while the rest prepared to move the patient to a gurney.
In the chaos, doctors didn't realize the wheel on the gurney was locked and wasted time fiddling.
Despite the hiccups, the patients survived in both cases.
© 2014 The Associated Press. All rights reserved.














