Obstructive sleep apnea treatments may reduce depressive symptoms
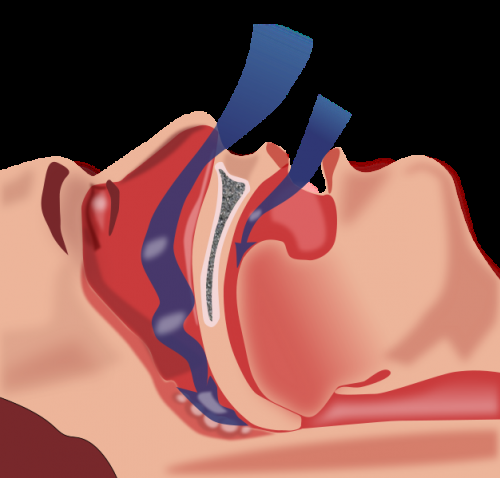
Treatment for obstructive sleep apnea with continuous positive airway pressure (CPAP) or mandibular advancement devices (MADs) can lead to modest improvements in depressive symptoms, according to a study published by Marcus Povitz, Carmelle Bolo, and colleagues from University of Calgary, Canada, in this week's PLOS Medicine.
The researchers identified 22 randomized controlled trials that investigated the effects of CPAP or MAD treatment on patients with obstructive sleep apnea and that measured depressive symptoms before and after treatment. By pooling the results from the 19 trials examining the effects of CPAP, the researchers observed that CPAP significantly improved depressive symptoms compared to the control intervention (usually sham-CPAP), with a greater improvements in those trials in which there was a higher prevalence of depression at baseline than in trials in which there was a low prevalence of depression at baseline. In a pooled analysis of the five trials that provided information about the effect of MAD on depressive symptoms, they observed that MAD also improved depressive symptoms compared to the control intervention (sham-MAD).
While the findings indicate that CPAP or MAD can lead to modest improvements in depressive symptoms among people with obstructive sleep apnea, they give no indication of the efficacy of CPAP and MAD compared to standard treatments for depression such as anti-depressant medications. Furthermore, the accuracy of the findings may be limited by methodological limitations within the trials included in the meta-analyses and, for the CPAP trials, there was considerable variability between trials.
The authors say: "this systematic review summarizes the available literature on OSA treatment, demonstrating that both CPAP and MAD treatment result in small improvements in depressive symptoms based on questionnaires. Our results illustrate that the greatest benefit of CPAP treatment on depressive symptoms may occur in populations with worse depression scores at baseline."
More information: Povitz M, Bolo CE, Heitman SJ, Tsai WH, Wang J, et al. (2014) Effect of Treatment of Obstructive Sleep Apnea on Depressive Symptoms: Systematic Review and Meta-Analysis. PLoS Med 11(11): e1001762. DOI: 10.1371/journal.pmed.1001762