Lowering risk of a major eye disease

Age-related macular degeneration (AMD), a chronic, progressive disease, is a leading cause of blindness among people aged 65 and older. Vision impairment due to advanced AMD significantly reduces quality of life and incurs substantial health care costs. Naturally, strategies to prevent AMD or delay its progression are important. Several Agricultural Research Service-funded scientists have been studying the possibility of reducing—by way of dietary modification—the risk of AMD.
"The promise of nutritional intervention was corroborated by two major clinical trials," says Allen Taylor, with the Jean Mayer USDA Human Nutrition Research Center on Aging (HNRCA) at Tufts University in Boston, Massachusetts. The two studies are known as the age-related eye disease studies. Named AREDS and AREDS2, the studies show use of a supplement containing vitamins C and E, lutein/zeaxanthin, and zinc delays the progression to advanced AMD in persons with intermediate AMD. The two AREDS studies were sponsored by the federal government's National Institutes of Health.
Now, for a study headed by HNRCA epidemiologist Chung-Jung Chiu, along with Taylor and coauthors, researchers analyzed existing data from AREDS and reported on how two U.S. dietary patterns they identified relate to the risk of AMD. Both Chiu and Taylor are with the HNRCA's Laboratory for Nutrition and Vision Research, which is headed by Taylor.

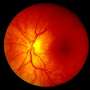
The macula is a 3-millimeter-wide group of light-sensing cells located at the back of the retina above the optic nerve. The macula's yellow color is due to pigments made up of plant chemicals called "carotenoids." An abnormal level of macular pigment is an early indicator of macular degeneration. In addition, as the eye ages, oxidized, damaged proteins and lipids—debris called "drusen"—begin to accumulate in the macula. This occurs when the damaged components are neither broken down by enzymes that control protein, lipid, and carbohydrate quality, nor detoxified via other mechanisms. Measurable drusen is another key indicator of AMD risk.
For the study, the team classified baseline data, which had been collected during AREDS on the eyes of more than 4,000 study volunteers, into three groups: The control group consisted of eyes having little or no drusen; the early-AMD group had eyes with intermediate or large drusen or with abnormalities in macular pigment; and the advanced-AMD group consisted of eyes with unusual blood-vessel growth or atrophy in the macula.
The researchers analyzed the participants' food-consumption data that had been already collected during AREDS via a 90-item food-frequency questionnaire. Two major food intake patterns emerged from this analysis—they were named "Oriental" and "Western." Those who adhered to the Oriental pattern consumed relatively high intakes of vegetables, legumes, fruit, whole grains, tomatoes, and seafood. Those who adhered to the Western pattern consumed relatively high intakes of red meat, processed meat, high-fat dairy products, French fries, and refined grains.
"The analysis showed that adherence to the Oriental pattern is associated with reduced odds of AMD," says Taylor. In contrast, people who consumed the Western pattern had markedly increased odds of AMD. "Our dietary-pattern analysis provides better insight into the diet–AMD relationship than a single-food or single-nutrient approach," says Taylor. This is because people eat groups of foods, not single nutrients. "The complex interactions among foods and nutrients are important."