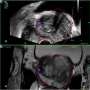
MRI—prostate cancer screening for the future?
A screening method that combines a traditional PSA test with an MRI detects a significantly greater number of prostate cancer cases and improves diagnostic accuracy. The study was conducted as part of the largest international research project on prostate cancer. The method will now be tried with 40,000 subjects in Gothenburg.
Prostate cancer, which is the third most common malignancy among European men, caused more than 92,000 deaths in 2012 alone.
Sweden and many other countries use the PSA test for diagnostic purposes. The test has been widely criticized for yielding false negatives, as well as false positives that lead to needless assessment and treatment.
As a result, Swedish authorities have not issued a general recommendation for PSA screening.
Improve detection
As part of a large European research project, scientists at Sahlgrenska Academy, University of Gothenburg, have studied a method that combines the PSA test with an MRI. Based on 384 Swedish subjects and presented in a doctoral thesis, the study concludes that the method can improve detection of more aggressive forms of prostate cancer.
"Additional research is required to confirm our findings, but the pilot study indicates that combining a PSA test with an MRI reduces the need for follow-up biopsies," says Anna Grenabo-Bergdahl, co-director of the study along with Professor Jonas Hugosson. "Depending on the PSA cut-off used, we can improve detection of potentially aggressive cancer while bypassing low-risk tumors that are generally of no clinical significance."
More precise biopsy
An MRI also facilitates identification of a possible malignant area such that any follow-up biopsy will be much more precise.
"That way the patient experiences less stress and clinicians are not as prone to overlook high-risk tumors," Dr. Grenabo-Bergdahl says.
The Swedish pilot study won the award for the best abstract by a resident at the Madrid conference of the European Association of Urology in late March.
Study on 40,000 subjects
The upcoming study will involve 40,000 subjects in the Gothenburg area.
"A repetition of the findings of the pilot study may be the opening shot of a paradigm shift in screening and early detection of prostate cancer," Dr. Grenabo-Bergdahl says.
Burden of unnecessary costs
The evidence is not in yet as to whether MRI is a cost-effective option for routine screening.
"Such an estimate must consider the costs associated with overdiagnosis under the current system," Dr. Grenabo-Bergdahl says.
"Many men who are diagnosed with prostate cancer on the basis of a PSA test are old enough that low-risk tumors will never pose any kind of danger to their health. Not only does the healthcare system bear the burden of unnecessary costs, but the patient's quality of life is compromised by worry and risky treatment. If the use of MRIs can help minimize such incidents while detecting more potentially aggressive tumors, it will represent genuine progress on all scores."
More information: The thesis is available online: gupea.ub.gu.se/handle/2077/38003