Dominant strain of drug-resistant MRSA decreases in hospitals, but persists in community
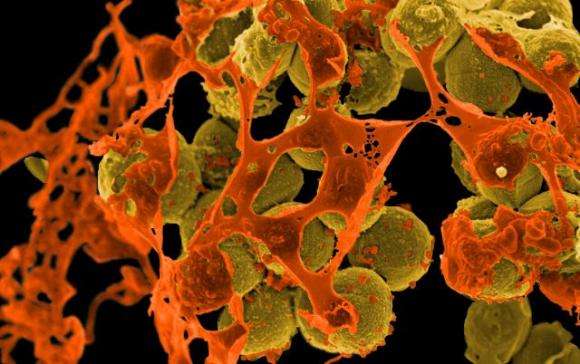
The incidence of the most common strain of Methicillin-resistant Staphylococcus aureus (MRSA) infections has decreased in hospital-onset cases, but has failed to decline in the broader community, according to new research published online today in Infection Control & Hospital Epidemiology, the journal of the Society for Healthcare Epidemiology of America.
The USA 300 strain of MRSA, has become prevalent in both communities and healthcare institutions. "In looking at risk factors for hospital or community-onset USA 300, current or former drug use was a strong predictor for acquiring this strain of bacteria," according to Kyle J. Popovich, MD, MS, the lead author of the study and Assistant Professor in the Section of Infectious Diseases, Rush University Medical Center, Chicago.
In the past 15 years, MRSA infections have evolved as the bacterium emerged as a significant pathogen in the community and hospitals in the U.S. Researchers studied 1,015 cases of Staphylococcus aureus bacterial bloodstream infections (BSI) over a six-year period at a Chicago "safety net" hospital. The study found that more than half of hospital-acquired cases were due to the USA 300 strain.
Recent national surveillance has suggested a decrease in the incidence of invasive hospital-acquired MRSA infections during the past decade, and researchers said their findings reaffirmed that observation in the Chicago region.
"Decreases in hospital-onset MRSA BSIs may be due to substantial efforts aimed to reduce healthcare-associated infection," said Popovich. "Enhanced prevention efforts in the community for certain populations, such as those engaging in illicit drug use, may be necessary to further curb the spread of invasive MRSA infections."
More information: Yoona Rhee, Alla Aroutcheva, Bala Hota, Robert A. Weinstein, Kyle J. Popovich. "Evolving Epidemiology of Staphylococcus aureus Bacteremia." Infection Control & Hospital Epidemiology, (September 16, 2015).