Big data in managing the future health of Singapore
Continuous data collection for chronic illness management is crucial to deliver personalized care for patients. In the era of globalization, patients still do not have the right tools to collect and share their physiological information on a frequent, real time basis. This becomes more crucial in scenarios where patients travel from regions of the world affected by epidemic diseases; e.g. Ebola in Africa, MERS in South Korea, and to travel as an infected host to other parts of the world.
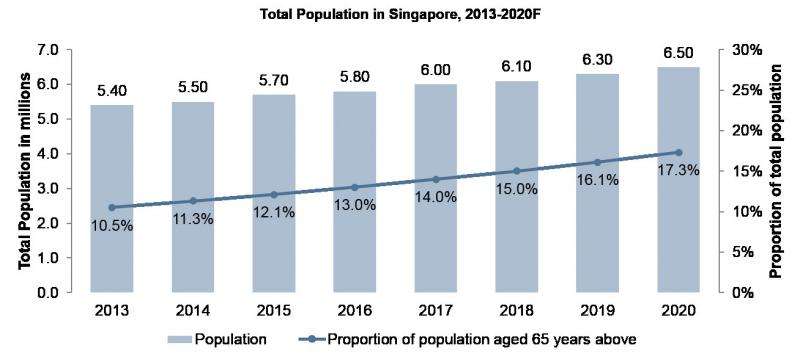
In Singapore, more than 48% of the disease burden is related to chronic diseases and the proportion of population aged 65 years and older is expected to increase in the next 10 years, Figure 1. Singapore is also heading towards a rapidly ageing society and this phenomenon is likely to increase the public's demand for better healthcare infrastructures and resources. Currently, most of the chronic diseases are managed in the primary-care system which is driven by a fee-for service model that emphasizes volume and profitability of services, e.g. General Practitioners clinics and polyclinics.
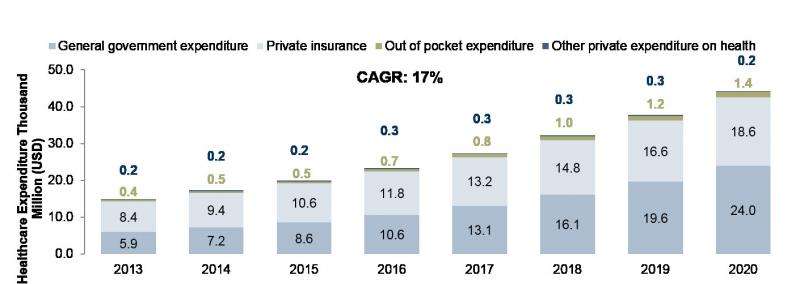
However, in next decade, the costs of medical services are expected to increase exorbitantly. Singaporeans will then require a better financial model to manage patients with chronic diseases and in a system where the doctors are paid a guaranteed sum per patient for a specified total population, Figure 2. This would provide incentives for all stakeholders towards managing patients' health status with little or no morbidity and at a minimal cost, which subsequently forms the basis for value-based healthcare. Big data and analytics are expected to play a major role in this market.
Singapore is one of the few countries in APAC, which has an electronic database to keep track of all hospital records. The purpose of health data management is to enable constructive assessments of clinical health outcomes and care quality and to ensure all medical treatments and health care are affordable to the public.
All these data are collectively termed as Big Data, needs to be consolidated and analyzed. Unlocking the hidden value in data and to translating numbers to meaningful information are expected to improve health care and attain better cost effectiveness in next 5-10 years. The value proposition of data analytics is expected to allow the policy makers to synthesize and discover patterns and correlations within the data that would not have been revealed otherwise.
Currently, there are early signs of players who are using big data to manage disease. TeleMetrix+ (TM+) is the first cloud-based commercial Telehealth service in Singapore. In this report we will consider some of the unique initiatives that are already in place and may scale up in next 5-10 years.
Disease Management Using Apps/IoT platforms
Recently one of the Singaporean companies "Healint" has reported a unique way of tracking data from patients suffering from migraine. The platform allows various healthcare stakeholders to take advantage of mobile devices, sensors, machine learning and big data for the optimal management of chronic diseases. Healint's first app Migraine Buddy has been listed as the number one most preferred migraine tracking app on Android devices in 2015, and the app has more than 100,000 users globally. Though in its initial phase the company has been successful in collecting extensive data from Migraine Buddy, it has reported the results of its first virtual study conducted on migraines. Currently the company is working with Khoo Teck Puat Hospital, Singapore to manage spinal stenosis using gait as a marker. The app is expected to leverage the historical data of patients with neurological disorders. It uses mobile sensor technology, and their analytics platform to better understand chronic conditions in an outpatient setting.
Singapore's Smart Health-Assist is an example of how ICM can enhance people's quality of life, improve work efficiencies, and create new growth opportunities using IoT infrastructure. The country already has a pervasive telecommunication infrastructure, and is expected to implement IoT infrastructure nationwide, soon. The same technology can also be used to create several Smart Home IoT ecosystem and add value to the users by offering services such as utilities or security. With a rapid ageing society this can not only help in quicker tracking of diseases, it will help doctors to monitor their seniors/bed ridden patients from the comfort of their homes.
Another example of remote patient monitoring services is "myHealth Sentinel". A monitoring service selected by Jurong Health in 2014 to implement a Medical Device Integration (MDI) solution for Ng Teng Fong General Hospital and Jurong Community Hospital, Singapore. MyHealth Sentinel also established partnership with National University Hospital and the Frontier Health Group in 2014, to deploy remote patient monitoring services to their chronic care outpatients.
The next five years will be interesting for clinicians and the general public in Singapore as more big data platforms are expected to be used in the healthcare market, and better apps will be available for disease management. Data gathered from these apps can help to better identify conditions such as stroke or patients who are at the highest risk of developing type-2 diabetes. If the data can help the policy makers to focus more on preventive measures on high risk individuals, then Big Data will show its charm and value as a cost-effective tool. It is expected that predictive analytics can stratify patients into different readmission risk categories that are based on their previous medical history, clinical markers, and demographic factors. More resources can be allocated to ensure high-risk patients receive frequent follow-up care and to reducing avoidable hospital readmissions.
More information: For more information, please visit: www.asiabiotech.com/19/1910/19100030x.html