February 25, 2016 report
Who is best to assess maternal and fetal risk?
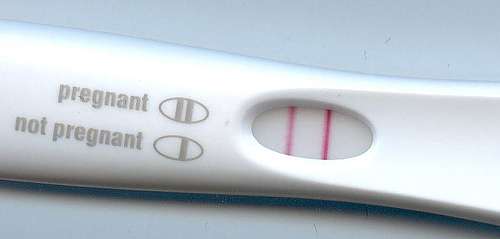
(Medical Xpress)—At what point does fetal risk outweigh maternal autonomy? The recent findings that the Zika virus may cause birth defects have lead some governments in Latin American countries to recommend that women not get pregnant until the virus can be contained. The Centers for Disease Control and Prevention have recently recommended that pregnant women or women who could become pregnant should not drink alcohol. Additionally, the increase in babies born to women addicted to drugs has caused some U.S. areas to punish pregnant women who use illicit substances while pregnant.
Minkoff and Marshall explore when and if the state or doctors should intercede on behalf of the fetus by forcing a woman to undergo a recommended procedure or treatment. They evaluate the nature of risk and how risk is used to justify punishing a mother for decisions made before the baby is born. They contend that many decisions regarding when it is appropriate to limit a pregnant woman's autonomy are based on subjective moral intuitions. They argue that it is ultimately up to the mother to make decisions in relation to the collective interest of her family. Their discussion and peer commentary responding to their paper appear in the recent issue of the American Journal of Bioethics.
Minkoff and Marshall begin their discussion by outlining the difference between absolute and relative risk and how relative risk can sometimes be used to justify preferences rather than assess actual risk thresholds. They use as examples a study on planned home births verses hospital births and a study of trial of labor after cesarean section (TOLAC). Reporting relative risk may involve saying a baby is twice as likely to die in a planned home birth as in the hospital, but absolute risk shows that the likelihood of a baby dying in a planned home birth is 1 in 1,000. The risk for both is low, but one is relatively higher than the other. TOLAC has a higher relative and absolute risk of infant mortality, but physicians are more likely to allow this than they are home births. The authors point out that a person's preconceived notions on a procedure may determine whether he or she considers the risk significant or not.
The American College of Obstetricians and Gynecologists and the American Academy of Pediatrics recognize that any intervention to help the fetus will have implications for the woman's bodily health and, therefore, cannot be performed without her explicit informed consent. While parents have a special obligation to their children Minkoff and Marshall take the view that even though the fetus has an evolving moral status during a voluntary continued pregnancy, parents do not have the same obligations as they do to born children.
They contend that the issue is less about the duty of the parent and more about the conduct of the state. On what basis can the state enforce coercive interventions that conflict with the mother's autonomy? Their examples from past cases as well as a survey among obstetricians indicate that the decision is based on motivated reasoning stemming from evolutionary-based intuitions on the developing fetus. Difficulties and disagreements occur in cases where these moral intuitions seems to conflict.
They conclude that while there may appear to be a conflict in moral intuitions, there actually does not have to be conflicts. The pregnant woman should be able to make decisions in relation to the collective interests of the entire family because it is her "personal, fetal, and family interests [that] hang in the balance." In other words, she considers the consequences to fetus and to herself within the context of the family or community.
There were several peer commentaries that provided comment or critique on Minkoff and Marshall's paper. They included discussions on the moral status of the fetus, gender biases and expectations, the subjectivity of determining risk, relational autonomy, cultural views on risk and pregnancy, racial biases in coerced care, as well as risk and religious obligations to fast.
More information: Howard Minkoff et al. Fetal Risks, Relative Risks, and Relatives' Risks, The American Journal of Bioethics (2016). DOI: 10.1080/15265161.2015.1120791
Abstract
Several factors related to fetal risk render it more or less acceptable in justifying constraints on the behavior of pregnant women. Risk is an unavoidable part of pregnancy and childbirth, one that women must balance against other vital personal and family interests. Two particular issues relate to the fairness of claims that pregnant women are never entitled to put their fetuses at risk: relative risks and relatives' risks. The former have been used—often spuriously—to advance arguments against activities, such as home birth, that may incur risk; the latter implicate the nature of relationships in determining the acceptability of coercing or precluding activities. Motivated reasoning by clinicians and judges leads to inaccurate risk assessments, and judgments based on false claims to objectivity. Such judgments undermine the moral and legal standing of pregnant women and do not advance the interests of fetuses, pregnant women, families, or states.
© 2016 Medical Xpress