Turning on blood flow turns on fat-burning brown fat in mice
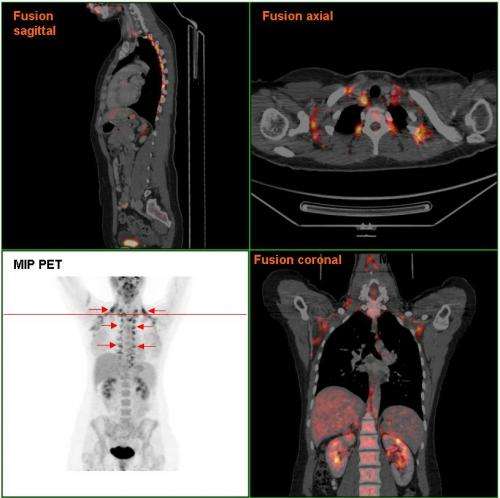
Increasing the blood flow in brown fat causes it to burn more calories in mice and may help treat obesity, a new study in the Journal of Applied Physiology reports.
The body has two types of adipose, or fat, tissue: white and brown. White fat stores energy. Obesity is characterized by too much white fat in the body. Brown fat uses energy to produce heat. It is associated with infants—it generates heat to keep infants warm because they cannot shiver—but it was recently found in adult humans as well.
Because brown fat uses energy, researchers are exploring if stimulating brown fat can use up and reduce the body's extra white fat. Drugs that directly stimulate brown fat activity, however, have significant side effects or have been shown to be ineffective treatments for obesity. Brown fat also has a large network of blood vessels within it. When brown fat is active and generating heat, blood flow increases to support it with enough oxygen and nutrients. This new study examined whether increasing blood flow can increase activity.
The researchers used salbutamol, a drug from the beta-2 adrenergic agonist drug class, to increase blood flow in the brown fat of normal-weight mice. They saw increased consumption of glucose (sugar), a sign of activity, by the brown fat. Salbutamol did not directly stimulate brown adipose cells, which suggests that the higher activity was due to the increased blood flow.
The findings have encouraging implications for patients because beta-2 adrenergic agonists are routinely used in clinical practice, including for asthma and pre-term labor, and have few side effects, according to the research team. The next step is to determine if chronically stimulating brown adipose tissue can help obese mice lose weight, said Laura Ernande, MD, PhD, and Marielle Scherrer-Crosbie, MD, PhD, lead authors of this study.
More information: Laura Ernande et al. Relationship of brown adipose tissue perfusion and function: A study through beta 2 adrenoreceptor stimulation, Journal of Applied Physiology (2016). DOI: 10.1152/japplphysiol.00634.2015