Reducing infectious malaria parasites in donated blood could help prevent transmission
A technique for reducing the number of infectious malaria parasites in whole blood could significantly reduce the number of cases of transmission of malaria through blood transfusion, according to a collaboration between researchers in Cambridge, UK, and Kumasi, Ghana.
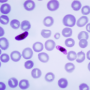
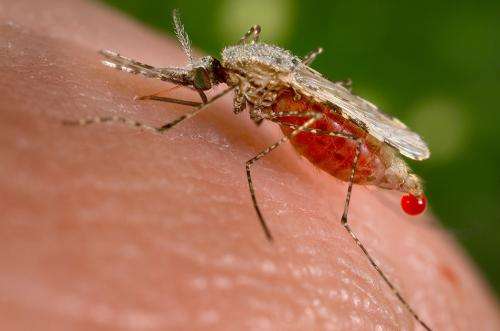
Malaria is a blood-borne disease caused by the malaria parasite - in west Africa, this is mainly Plasmodium falciparum. The parasite is mainly transmitted to humans through mosquito bites. In sub-Saharan Africa, malaria infection is endemic and a substantial proportion of the population carries the parasite, even when individuals do not show any symptoms. Only a few blood centres screen donor blood of the parasite and hence there is a high risk of malaria transmission through transfusion.
Because of resource limitations, the most common red blood cell product transfused is whole blood. A half of all blood donors in Ghana carry detectable levels of malaria parasites in the blood and as many as one in four (between 14-28%) of blood recipients become infected.
The Mirasol pathogen reduction technology system, developed by the US-based Japanese company Terumo BCT, has been developed to treat whole blood using ultraviolet light energy and riboflavin (vitamin B2) to reduce the parasite load and to inactivate white blood cells. It has been shown to reduce P. falciparum load in vitro and to maintain adequate blood quality during 21 days of cold storage.
In a study published today in The Lancet and funded by Terumo BCT, researchers report the results of the African Investigation of the Mirasol System (AIMS) trial, which explored whether the use of blood treated with Mirasol would prevent the transmission of malaria to patients with anaemia being supported with whole blood transfusion.
"In developing countries, blood supplies are often contaminated and blood banking systems cannot afford the newest technologies for detecting blood-borne pathogens," explains Professor Jean-Pierre Allain from the Department of Haematology at the University of Cambridge. "Technologies aimed at reducing the levels of parasites or infectious agents in the blood could benefit individual patients and also health-care systems."
The trial involved 214 patients, 107 of whom received Mirasol-treated blood, the remainder of whom received the normal blood products. Overall, 65 patients who previously were free of detectable parasites were transfused with blood retrospectively found to contain parasites - 28 of these blood products had been treated with Mirasol, 37 were untreated.
The incidence of transfusion-transmitted malaria was significantly lower for those patients who received the treated blood (one out of 28 patients, or 4%) compared to the untreated group (eight out of 37 patients, or 22%).
At the same time, the safety profile did not differ for patients receiving treated or untreated whole blood units. The treated whole blood group had fewer allergic reactions to the transfusion (5% vs 8%) and fewer overall reactions (8% vs 13%), possibly because of the technology also inactivates white blood cells including immune cells.
The researchers recognise that the overall number of transmissions was small, reducing the power of the study, but believe it still provides a clear indication that the Mirasol system could make a dramatic difference to the number of cases of malaria transmission via blood transfusion.
"This could be a real game-changer for blood safety in sub-Saharan African," adds Dr Shirley Owusu-Ofori from the Transfusion Medicine Unit, Komfo Anokye Teaching Hospital, Kumasi, Ghana. "Reduced transfusion-transmissions of infectious agents means a more stable blood supply, reduced costs for the treatment of preventable infections, and direct benefits to women and children who are especially vulnerable to malaria."
More information: Allain, JP et al. Effect of Plasmodium inactivation in whole blood on the incidence of blood transfusion-transmitted malaria in endemic regions: the African Investigation of the Mirasol System (AIMS) randomised controlled trial. Lancet; 23 April 2016.