Threshold for pre-emptive surgery to curb ovarian cancer risk should be halved
The current threshold for pre-emptive surgery to remove the ovaries and fallopian tubes of women aged 40+ at high risk of developing ovarian cancer should be halved, concludes research published online in the Journal of Medical Genetics.
This would not only extend the lives of more women, but would be very cost effective, and help to compensate for the current lack of a reliable test to screen for the disease, suggest the researchers.
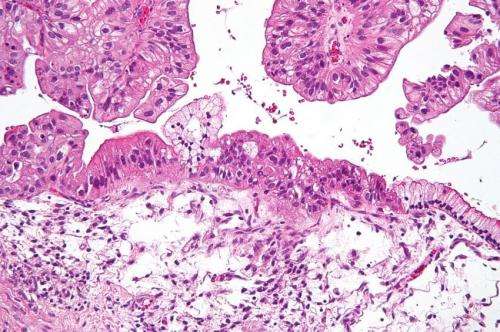
Ovarian cancer remains the leading cause of cancers affecting the reproductive system among women. Globally, it kills 152,000 of them every year.
Pre-emptive surgery, known as risk reducing salpingo-oophorectomy, is the best option for curbing ovarian cancer risk among women at high risk of developing the disease. These include those with a first degree relative affected by the disease and carriers of risk genes, such as BRACA1/2 , and to a lesser extent, RAD51C, RAD51D, and BRIP1 genes.
But the procedure is currently only available to women with at least a 10% lifetime risk of developing the disease, a threshold that has never been tested for its cost effectiveness.
The researchers therefore decided to compare the costs and effectiveness of pre-emptive surgery with no surgery for women aged at least 40 who had not yet gone through the menopause, but who were at risk of developing the disease, using mathematical modelling.
Different levels of lifetime risk were included in the analyses—2%, 4%, 5%, 6%, 8% and 10%—to calculate the likelihood of developing ovarian cancer, breast cancer, and death from heart disease.
Costs were derived from official sources at 2012 prices and average life expectancies for women with and without breast or ovarian cancer were taken from national statistical data to calculate Quality Adjusted Years or QALYs for short—a measure of years lived in good health.
When all the data were analysed, the calculations showed that pre-emptive surgery at a lifetime risk level of 4% or greater would be highly cost effective among women aged at least 40, and add up to around 43 extra days of life expectancy if hormone replacement therapy were taken until natural menopause.
"Our results are of major significance for clinical practice and risk management in view of declining genetic testing costs and the improvements in estimating an individual's ovarian cancer risk," write the researchers.
"With routine clinical testing for certain moderate penetrance genes around the corner and lack of an effective ovarian cancer screening programme, these findings are timely as they provide evidence supporting a surgical prevention strategy for 'lower risk' individuals," they conclude.
More information: Specifying the ovarian cancer risk threshold of 'premenopausal risk-reducing salpingo-oophorectomy' for ovarian cancer prevention: a cost effectiveness analysis, Journal of Medical Genetics, DOI: 10.1136/jmedgenet-2016-103800