'Lifelike' human body to help train surgeons
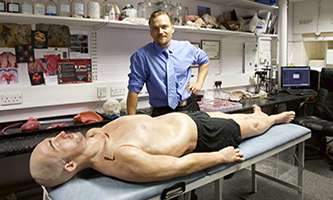
A researcher has used 3-D printing to create an imitation human body with the tactile qualities of living organs to train surgeons dealing with trauma emergencies.
Richard Arm – of Nottingham Trent University's School of Art & Design – working alongside industry partners, created the model from silicone gels and fibres to help prepare trainee surgeons for the mental and physical experience of operating on chest cavity organs.
The research – which is in collaboration with the Ministry of Defence's (MoD) Royal Centre for Defence Medicine, Professor Michael Vloeberghs, Neurosurgeon at the Queens Medical Centre in Nottingham, and other industry partners – uses CT scans of real organs to create lifelike simulations of the heart, lungs and great vessels in the chest.
The outer skin – created by Yorkshire-based Trauma FX – uses a lifecast of an anonymous model and can be cut into with a scalpel and seamlessly resealed to allow for repeated mock surgeries.
"The aim is to allow trainee surgeons the psychological space to prepare for real life surgery using immersive environments and realistic representations of human anatomy," explains Richard, a research fellow and PhD candidate at the University.
"By communicating the experience of performing cardiothoracic surgery, surgeons can be better prepared for live surgery by improving their surgical skills and enhancing post-operative outcomes for patients."
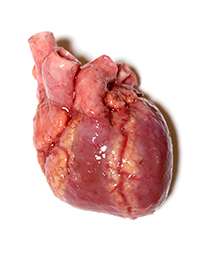
The imitation organs provide tactile simulations of living tissue by varying in hardness – such as around a heart's blood vessels – to give a realistic feel.
A limited supply of artificial blood can be pumped into the body to provide the experience of operating against the clock, before a fatal level of blood-loss occurs.
Because internal and external details are included the model can even be ventilated – to give a realistic simulation of a patient breathing – using medical standard ventilators, allowing surgeons to see the movement of the patient's chest as he or she breathes.
The prototype (pictured) is set to go on public display at Trauma Innovation 2016, hosted near Birmingham on 27 and 28 September. Surgeons will provide feedback on the prototype before two models are then produced for the MoD by December 2017.
The research will also explore how future models can be made cost-effective, with higher and lower spec body parts for different types of training scenarios.
Plans are being made to expand the research to create other lifelike organs including the brain, eyes, stomach, pancreas, liver and kidneys, and the vascular system in a person's legs as well as bespoke models for patient-specific preoperative surgical planning.

Colonel Peter Mahoney CBE, Emeritus Professor of Anaesthesia, Defence Medical Services, said: "This is a really exciting and innovative collaboration with Nottingham Trent University.
"The ability to place clinically realistic surgical and anaesthetic training models into simulations of austere military environments is of great value to military medicine.
"As well as providing a training platform for our surgical teams, the thoracic trauma trainer will be of benefit to our prehospital Medical Emergency Response Teams."
Professor Tilak Dias, a supervisor of the project at Nottingham Trent University, said: "Richard's work shows how art and science can be combined to improve the way critical surgery is performed.
"By enhancing the learning experience of surgeons, we can ensure they are better prepared for real life situations where their skills and knowledge are relied upon to save people's lives."


















