Patients eager to test device that could ease heart failure symptoms

Jimmy McMillan doesn't know if it's science or wishful thinking that's making him feel better, but he's starting to believe a round of golf is in his future, something that seemed impossible a few months ago.
"I told Dr. Litwin, 'I don't know if I have the device or not, but if I don't, I have one heck of a placebo effect.'"
It's no surprise that McMillan, a participant in a clinical trial testing a heart failure treatment device at MUSC Health, hopes things are getting better. The former sales manager for a medical products company, now on medical disability leave, has been through a lot since his heart problems began several years ago.
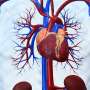
Like more than five million other Americans, McMillan has heart failure. But unlike the more widely known type of heart failure in which the heart has reduced pumping ability, McMillan's symptoms result from his heart's inability to fill with blood at normal pressures. It's called as heart failure with preserved ejection fraction, or HFpEF. It causes shortness of breath, tiredness and swelling. It used to be called diastolic heart failure.
For some patients, it's easier to think of the disease as "huff puff" because of the way it affects their breathing. The culprit is elevated pressure in the left atrium of the heart. It leads to repeated hospitalizations, the inability to do routine tasks and in some cases, sleeping in a chair to breathe comfortably. There are no medications known to slow its progression.
The MUSC Health Cardiology team has doctors who specialize in treating this challenging condition and researching better treatments. One of them, Sheldon Litwin, M.D., is leading MUSC's part of the multi-site trial called Reduce LAP (left atrial pressure) that McMillan is taking part in. It's testing the Corvia Medical InterAtrial Shunt Device.
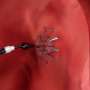
Previous research on the device published in The Lancet was promising, Litwin said. The MUSC professor and SmartState Countess Alicia Spaulding-Palozzi Endowed Chair in Cardiovascular Imaging said the device makes a small hole, about the width of a pencil, between the upper chambers of the heart to redistribute blood and reduce the pressure on the left side and lungs.
"If you can create a hole of that size, they reasoned that left atrial pressures would be lower, people would breathe better and even if there's extra pressure on the right side, that tends to cause edema or swelling in the feet," Litwin said.
"Which would you rather have? Can you live with some swelling in your feet, or can you live with not being able to walk across the room? So if comes to a tradeoff, a little bit of right heart failure would be better."
McMillan agrees. On a recent afternoon, he came to MUSC Health for a checkup with Michael Zile, M.D., another HFpEF specialist. Neither McMillan nor Zile knows if McMillan is in the group of patients who got the device or if he's in the control group. They're "blinded." That's intentional, to protect the integrity of the trial.
"How far can you walk?" Zile asked McMillan.
"I can walk for 15 minutes on a treadmill at 2.4 miles an hour," McMillan answered. "With a slight incline."
"The fact that you can walk like that is great," Zile said.
"I seem to have more energy. I'm still short of breath, but the recovery is a little better," McMillan said. "The symptoms seem to be better controlled. I've been able to come off some my pain meds and diuretics and blood pressure medication has been reduced a little bit.McMillan said he's grateful to the HFpEF team at MUSC Health for taking care of him and giving him hope. Because HFpEF is so difficult to treat, some doctors elsewhere aren't sure what to do with these patients, Litwin said.
"These patients have lots of symptoms, they come back a lot, they're hospitalized a lot. Nobody wants to take care of them because they're hard to care for. Everybody's under the gun about heart failure readmissions. We get penalized by Medicare if somebody's hospitalized here and then gets re-hospitalized again within 30 days. It's a huge thing right now," Litwin said.
"So patients have a hard time finding somebody interested in their disease.
There are very few places around country that really say, 'This is an important problem. This is my specialty. This is what I do.'"
Heart doctors tend to focus on people with another type of heart failure, systolic dysfunction, because they're candidates for heart transplants and left ventricular assist devices. "These HFpEF patients are not felt to be candidates for those things. But at MUSC Health, we want to see these patients because we feel that we have several different novel treatments to offer them," Litwin said.
McMillan will find out at the end of a year if he has the Corvia Medical InterAtrial Shunt Device implanted or not. If he didn't, and he wants one, he can get one then.
"I'll never be able to walk a course again, but if I could use a golf cart and play a round of golf, at least nine holes, I'd love it. I've gone to hit a few golf balls but I have to rest. I'm still not where I want to be.
"And if I could not feel quite so helpless around the house. I was the type person who did everything. It's been quite a challenge to have to sit back and accept help on everyday tasks."
Litwin wants McMillan and others with HFpEF to enjoy a return to a higher quality of life. "We're interested in trying to understand the disease, to be pioneers in new therapies and offer new options to patients. We're really the only ones in South Carolina who are doing this."
The Reduce LAP trial is one of four studies involving HFpEF patients underway at MUSC Health. The others involve:
- Weight loss management for people with HFpEF, which is linked to obesity
- The Paragon HF trial, testing whether an investigational heart failure medicine by Novartis works in patients with HFpEF
- A trial testing whether heart stem cells can be used to reprogram malfunctioning cells in people with HFpEF