March 31, 2017 report
Study shows prior viral infections can make Zika infection worse
(Medical Xpress)—A team of researchers with the Icahn School of Medicine at Mount Sinai in New York City has found that mice who have survived a dengue or West Nile viral infection fare worse when subsequently infected with the Zika virus compared to those that have not had such prior infections. In their paper published in the journal Science, the team explains how they tested human plasma in lab dishes and in mice to learn more about the possible implications of Zika infections in people who have previously experienced other viral infections.
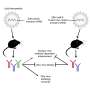
Prior research has shown that oftentimes when a person survives a dengue infection, they fare worse with a second dengue infection if it is a different kind. When humans and mice become infected with a virus, the body creates antibodies as a response. Such antibodies help protect against future infections. But in some cases, those same antibodies can cause a host to be less protected against a different virus from the same family due to an antibody-dependent enhancement reaction, which can leave those with initial infections at greater risk from secondary infections. In this new effort, the researchers looked at the possible implications of such reactions regarding Zika, because it is related to both dengue and West Nile.
The team ran two kinds of tests. In the first series, plasma samples were obtained from people who had been infected with dengue or West Nile and from people who had never had any related infections. The researchers found that when Zika was introduced to the plasma, it bound to the antibodies of those who had experienced dengue and West Nile infections (which meant it was more able to infect cells) but not to the antibodies of those that had never had either infection.
In the second series of tests, the researchers injected the plasma samples (simulating prior infections) into mice and then watched to see what would happen after they were infected with Zika. They report that the survival rate for mice given plasma from a dengue infected person was just 20 percent, for West Nile it was 60 percent and for those that received plasma from donors who had never been infected the survival rate was 93 percent.
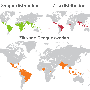
The researchers note their results are alarming because dengue is widespread in many parts of South America where Zika is spreading, and the same is true for West Nile in North America. The team plans to continue their studies looking for real-world cases of people infected with Zika who have experienced prior infections from dengue or West Nile to see if they fared worse.
More information: Susana V. Bardina et al. Enhancement of Zika virus pathogenesis by preexisting antiflavivirus immunity, Science (2017). DOI: 10.1126/science.aal4365
Abstract
Zika virus (ZIKV) is spreading rapidly into regions around the world where other flaviviruses, such as dengue (DENV) and West Nile virus (WNV) are endemic. Antibody-dependent enhancement (ADE) has been implicated in more severe forms of flavivirus disease, but whether this also applies to ZIKV infection is unclear. Using convalescent plasma from DENV and WNV infected individuals, we found substantial enhancement of ZIKV infection in vitro that was mediated through IgG engagement of Fcγ receptors. Administration of DENV or WNV convalescent plasma into ZIKV-susceptible mice resulted in increased morbidity and mortality, including fever, viremia, and viral loads in spinal cord and testes. ADE may explain the severe disease manifestations associated with recent ZIKV outbreaks and highlights the need to exert great caution when designing flavivirus vaccines.
© 2017 Medical Xpress