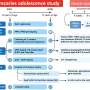
Dentists in good compliance with American Heart Association guidelines, according to Rochester epidemiology project
In the first study examining dental records in the Rochester Epidemiology Project, results show that dentists and oral surgeons are in good compliance with guidelines issued by the American Heart Association (AHA) in 2007, describing prophylactic antibiotic use prior to invasive dental procedures.
The Rochester Epidemiology Project is a collaboration of medical and dental care providers in Minnesota and Wisconsin. With patient agreement, the organizations link medical, dental, surgical procedures, prescriptions, and other health care data for medical research.
Prior to 2007, the AHA guidelines recommended prophylactic antibiotics for patients with cardiac conditions who were at moderate or high risk of developing infective endocarditis—a potentially deadly infection of the heart valve. After 2007, AHA recommended that only high-risk patients receive the antibiotics. This group represents a very small fraction of the individuals receiving antibiotics before 2007, says Daniel DeSimone, M.D., study lead author and infectious diseases and hospital internal medicine physician at Mayo Clinic. The study will be released May 23 online in Mayo Clinic Proceedings.
Earlier studies by Dr. DeSimone's team determined the incidence of infective endocarditis in Olmsted County before and after 2007, using Rochester Epidemiology Project data. They found no significant increase in cases of infective endocarditis following the introduction of updated AHA guidelines.
However, "the major limitation of these studies was the lack of access to dental records," says Dr. DeSimone.
"The inclusion of dental records in the Rochester Epidemiology Project provides a unique opportunity unlike any population health database in the United States," he says.
"The primary criticism of the earlier studies was, 'Are dentists actually following the 2007 AHA guidelines, or do patients continue to receive antibiotics when no longer indicated?'" reports Dr. DeSimone. "How could we prove that dentists were actually following the guidelines, rather than assuming they were? Now we can."
Dr. DeSimone also says, there are a number of health risks for patients when taking antibiotics. "Plus overuse of antibiotics can result in increased bacterial resistance, which is a widespread public health problem," he says.
In addition, while the cost to patients might only be a few dollars a dose, Dr. DeSimone says that when added up, this group of moderate-risk patients could spend well over $100 million per year.
"Using the Rochester Epidemiology Project, we have shown that the new guidelines were very helpful in reducing unnecessary antibiotic use and related issues, without an increase in new cases of infective endocarditis."
Although this was the first study using the newly linked dental records, it was just one of more than 2,600 medical research publications using the Rochester Epidemiology Project. Using medical and dental records, researchers can identify what causes diseases and how patients with certain diseases respond to surgery, medication or other interventions. They also can determine what the future holds for patients with specific diseases or medical conditions.
In another article published in BMJ Open, Alan Carr, D.M.D., chair of Dental Specialties at Mayo Clinic, and other authors describe the purpose of adding dental records to the Rochester Epidemiology Project data.