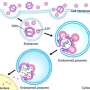
Researchers explore a new way of specific drug delivery using liposomes
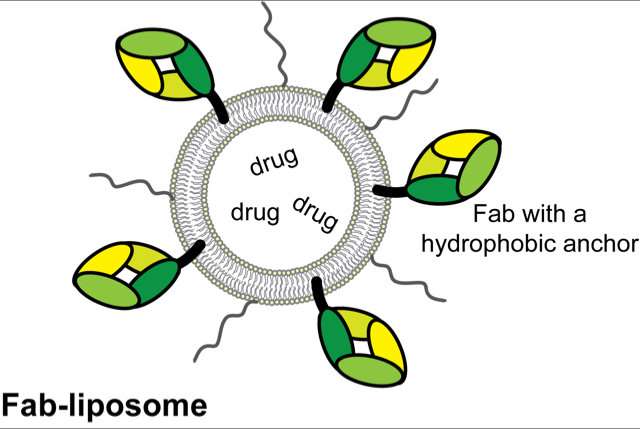
Liposomes are successful drug delivery vehicles prescribed for several types of cancer but also for treatment of fungal infections or pain management. Now researchers from the Medical University of Vienna show a straightforward method to functionalize liposomes for specific targeting, potentially paving the way to personalized medicine. The study has now been published in Nanomedicine: Nanotechnology, Biology, and Medicine.
The concept of liposomal drug delivery has revolutionised the pharmaceutical field and came into practice some 20 years ago when the first liposomal formulation of the anti-cancer drug doxorubicin was approved for clinical use. Liposomes, <200 nm phospholipid vesicles, are longer retained in blood circulation and accumulate at pathological sites (tumours or inflamed tissues), leading to higher efficacy and lower systemic toxicity compared to the free drugs they encapsulate. To target liposomes to certain tissues or cells, such as tumour cells, a specific binder of a unique protein (an antigen) on the targeted cell, known as a monoclonal antibody, must be linked to the liposome surface. This coupling is called the functionalization of the liposome and done chemically, often at the final stages of liposome production and can potentially damage the liposome or targeting antibody.
The new study by Anna Ohradanova-Repic and colleagues from the Medical University of Vienna, in collaboration with the University of Minho in Braga, Portugal, shows an easy method for liposome functionalization: They linked the small specific fragment of the antibody, called Fab, with a hydrophobic anchor. Via this hydrophobic anchor, the Fab fragment is naturally inserted into the hydrophobic liposomal membrane part during liposomal preparation. "It was quite fascinating to see how easy the liposome functionalization was. We tested two different Fab fragments and they both worked very well. We observed specific targeting not only to the antigen-positive cells in the lab dish but also in mice, where our liposomes precisely recognized human tumours that we had implanted," says Anna Ohradanova-Repic, the leading researcher behind the study.
Hannes Stockinger, the senior author of the study, says, "If we coupled this delivery method with screening of patient's tumours for the presence of a unique surface protein, which we can target with the Fab fragment-functionalized liposomes, we might be able to treat tumours more efficiently and decrease the side effects of the delivered anti-cancer drugs substantially. I foresee this as a personalized medicine of the future. Yet, a lot of work is ahead of us to implement this treatment strategy in clinical practice."
More information: Anna Ohradanova-Repic et al. Fab antibody fragment-functionalized liposomes for specific targeting of antigen-positive cells, Nanomedicine: Nanotechnology, Biology and Medicine (2017). DOI: 10.1016/j.nano.2017.09.003