Study points to potential personalized approach to treating lupus
In individuals with lupus, immune cells attack the body's own tissue and organs as if they are enemy invaders. A new Yale-led study describes how a protein found in common bacteria triggers that auto-immune response. The finding opens the door to future therapies targeting the bacteria rather than the immune system, the researchers said.
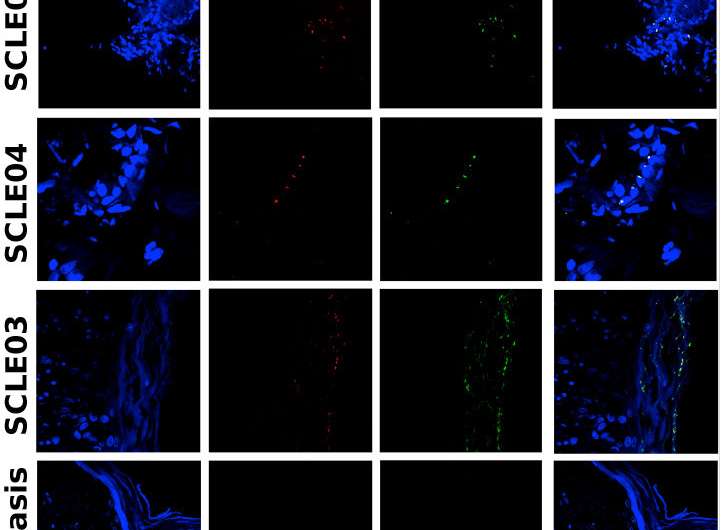
To deepen understanding of the autoimmune response generally, a research team lead by co-senior authors Martin Kriegel and Sandra Wolin, focused on a protein, Ro60, that has been found in lupus patients even before they developed symptoms. The protein induces the immune response and production of antibodies. In the study, the research team tested blood and tissue samples from patients with the most common form of the disease, systemic lupus. They identified Ro60 in bacteria from different parts of the body, including the mouth, skin, and gut.
The researchers theorized that the bacteria triggers an autoimmune response, which over time spreads to affect even healthy tissue. This chain of events leads to full-blown autoimmunity and lupus, Kriegel said.
More research is needed but the new insight could lead to the development of personalized treatments for autoimmune disease, he noted. For example, a topical medicine could be designed to target bacteria in the skin or other organs where autoimmunity manifests.
More information: Teri M. Greiling et al. Commensal orthologs of the human autoantigen Ro60 as triggers of autoimmunity in lupus, Science Translational Medicine (2018). DOI: 10.1126/scitranslmed.aan2306














