Telemonitoring in cardiac disorders: Benefit still unclear
To prevent cardiac death, people with certain cardiac disorders are implanted with electronic devices designed to automatically stimulate the heartbeat or counteract serious arrhythmia if necessary. Nowadays these devices also permit to monitor heart function from a distance. In case of conspicuous recordings, the physician may take additional therapeutic measures.
However, it remains unclear whether this so-called telemonitoring has advantages for patients with cardiac failure or heart rhythm disorders with a fast heart rate (ventricular tachyarrhythmia). This is the conclusion reached in the final report of the German Institute for Quality and Efficiency in Health Care (IQWiG).
Data on adverse events and quality of life are still lacking because only incomplete study results have been published. Even IQWiG's public request did not change this. Regarding other outcome criteria, treatment results with telemonitoring were neither better nor worse than without telemonitoring.
Electrical impulses to stabilize cardiac function
Cardiac failure is a common disease, particularly in older people and is one of the most common causes of death in Germany. So-called ventricular tachyarrhythmia is common in cardiac failure. Tachyarrhythmia is a combination of a heart rhythm disorder (arrhythmia) and a fast heart rate (tachycardia) that starts in one of the two lower chambers of the heart (ventricles). In the worst case, it can cause sudden cardiac death.
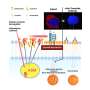
Both diseases are treated by implanting the patients with active cardiac devices. If the heartbeat is irregular, the devices transmit electronic impulses to either give defibrillation shocks or cause overstimulation (ICDs), or synchronize the contraction of left and right ventricle (CRTs). A third type of device combines both functions (CRT-Ds).
Telemonitoring to support follow-up care
Irrespective of the type of implant, regular (outpatient) follow-up care is necessary, where patients have to visit their physician at fixed intervals of usually three months. In principle, all types of devices nowadays also permit so-called telemonitoring. With telemonitoring, physiological data are radio-transmitted to the practice or to another medical centre and monitored. If necessary, visits independent from the regular follow-up visits can be scheduled to initiate diagnostic or therapeutic interventions. Telemonitoring is also designed to partly replace visits to the physician, however.
No relevant differences in most outcome criteria
A comparatively broad database - for non-drug interventions - had been available to the Institute already for the preliminary report. One further study was found in a search update. A total of 17 studies with 10 130 participants were now included in the assessment. Participants in these studies received either standard follow-up care alone or additional telemonitoring.
For most outcome criteria, the data showed no or no relevant differences between both treatment groups. This was the case for mortality and occurrence of strokes or heart attacks as well as for hospitalizations or occurrence of mental problems.
Particularities in the study design of IN-TIME
Yet there was one exception: One of the 17 studies (IN-TIME) produced results in favour of telemonitoring regarding mortality (all-cause mortality and cardiovascular mortality). The design of the IN-TIME studies was particular, however: On the one hand, the participants were monitored more closely than in the other studies included. On the other, follow-up care in the control group was less intense compared with the usual care in Germany: The first time the patients had to see their physician for examination was only after 12 months.
It therefore remains unclear whether the results of IN-TIME were caused by the particularly close monitoring in the telemedicine group or by the - compared with other studies - less frequent follow-up visits in the control group. The Institute therefore derived no benefit from the IN-TIME study either.
Quality of life: no data from 82% of study participants
In the overall consideration of the studies, still no conclusions can be drawn on benefit or harm for two key outcomes, namely side effects and quality of life, because data were missing for a considerable proportion of the patients.
Regarding serious adverse events, including side effects of the treatment, no results were available for 42% of the participants. This proportion was as high as 82% for health-related quality of life.
It would be inadequate to only include those participants in the assessment for whom data are available because the probability of a biased result is very high if such a large proportion of data is missing.
Several studies still unpublished
Data of study participants are not the only information that was missing, however. Three studies that are probably relevant for the assessment were not yet published at the editorial deadline. In addition, IQWiG identified five more completed studies that were not yet published. Their relevance was unclear, however. The EVATEL study was one of these studies: It was completed more than six years ago, but only an abstract has become available since.
Although IQWiG had criticized this fact before the commenting procedure, neither the manufacturer nor the study authors from publicly financed institutions subsequently provided data. "Particularly the industry has wasted the opportunity to show a benefit of their devices", says Stefan Lange, IQWiG's Deputy Director. "Clinical studies are not an end in themselves, but all their results have to become publicly available as quickly as possible. This is the only way for us to be able to assess the benefit and harm of the medical interventions. And without this knowledge, patients are not able to make informed decisions", he adds.
Process of report production
IQWiG published the preliminary results in the form of the preliminary report in August 2017 and interested parties were invited to submit comments. At the end of the commenting procedure, the preliminary report was revised and sent as a final report to the commissioning agency in January 2018. The written comments submitted are published in a separate document at the same time as the final report. The report was produced in collaboration with external experts.
More information: www.iqwig.de/en/projects-resul … rt-failure.7436.html