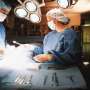
Outdated surgical choices put women at risk
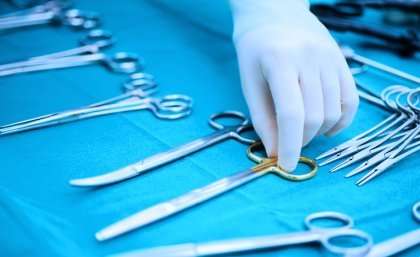
Australian women are undergoing unnecessarily invasive hysterectomies due to a lack of contemporary surgical skills among gynaecologists.
University of Queensland research has found many gynaecologists have not updated their skills, despite evidence supporting less invasive procedures.
Queensland Centre for Gynaecological Cancer Research Director Professor Andreas Obermair said many gynaecologists recognised the advantages of laparoscopic (keyhole) hysterectomy, but a lack of training meant many could not perform the procedure.
"Overwhelming evidence suggests that laparoscopic hysterectomy has better patient and societal benefits than traditional open hysterectomy," he said.
"The procedure is associated with a shorter hospital stay, quicker recovery, better quality of life and less cost to the health care system.
"However, we found surgeons were choosing to perform open hysterectomies instead because they were very experienced in that—essentially they were comfortable doing what they've always done."
Open hysterectomy involves the removal of the uterus and potentially all reproductive organs via a large cut.
A laparoscopic hysterectomy is a minimally invasive keyhole surgical procedure using three or four incisions no longer than six millimetres.
Professor Obermair said the study also found that laparoscopy workshops failed to provide adequate training.
"These workshops don't really teach them how to do this operation and, as specialists, there's no regulatory need to update their surgical skills," he said.
"A trainee learns all the time, they're used to it, but once you're a specialist there's this expectation from society that you know it all."
The study has informed a program funded by the National Health and Medical Research Council aimed at updating the surgical skills of gynaecologists in Queensland.
"We are now training 10 specialists so that they're able to reduce the use of open hysterectomies and offer less invasive alternatives," Professor Obermair said.
An initial test program at one hospital in the greater Brisbane area saw doctors choose laparoscopic hysterectomies over open hysterectomies in the majority of cases, with surgical complication rates falling by one-third.
The research is published in the Australia and New Zealand Journal of Obstetrics and Gynaecology.
More information: Monika Janda et al. Surgical approach to hysterectomy and barriers to using minimally invasive methods, Australian and New Zealand Journal of Obstetrics and Gynaecology (2018). DOI: 10.1111/ajo.12824