Trial finds no benefit of bath emollients beyond standard eczema care for children
Emollient bath additives provide no meaningful benefit when used in addition to standard eczema care in children, finds a trial published by The BMJ today.
Bath additives are widely prescribed at a cost of more than £23m ($33m; €26m) annually to the NHS in England. The researchers say their findings may help guide decisions around effective prescribing in this area.
Eczema (also known as atopic eczema or atopic dermatitis) is the most common inflammatory skin condition in childhood and can have a substantial impact on patients' and families' quality of life and NHS resources.
Emollients are the mainstay of treatment, providing a barrier over the skin, reducing moisture loss, and protecting against skin irritants. There are three methods of application of emollients; leave-on emollients, soap substitutes and emollient bath additives.
Although evidence supports the use of leave-on emollients and there is clinical consensus around soap substitutes, little good evidence exists on the benefits of emollient bath additives.
So a team of UK researchers, led by Miriam Santer at the University of Southampton, set out to determine both the clinical and cost effectiveness of including emollient bath additives in the management of eczema in children.
The trial included 482 children (244 girls / 238 boys) aged 1-11 years diagnosed with eczema from 96 general practices in England and Wales. Most participants had moderate eczema.
Children were randomly assigned to two groups. For one year, children in the intervention group were prescribed one of three bath additives, while the control group was asked to use no bath additives.
All participants received written instructions to use leave-on emollients as soap substitutes. They were advised to continue all other eczema care as usual, including regular use of leave-on emollients and corticosteroid creams as required.
Eczema control was measured weekly for 16 weeks using the patient oriented eczema measure (POEM, scores 0-7 mild, 8-16 moderate, 17-28 severe).
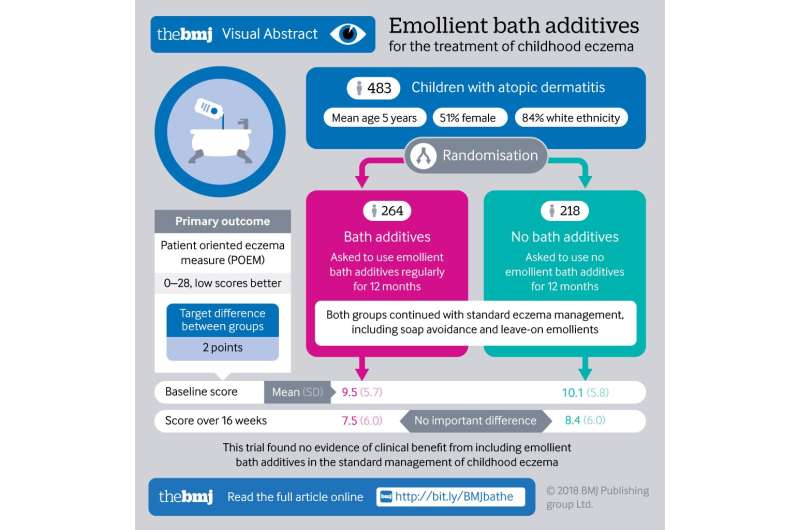
The researchers found no statistically significant difference in weekly POEM scores between the two groups over the 16 week period (mean POEM score of 7.5 in the bath additives group and 8.4 in the no bath additives group).
After taking account of eczema severity and other factors that could have affected the results, the POEM score in the no bath additives group was 0.41 points higher than in the bath additives group over 16 weeks, which is substantially lower than the minimal clinically important difference for POEM of 3 points.
There were also no significant differences between the two groups for additional measures, including eczema severity over one year, number of eczema flare-ups, quality of life, cost effectiveness, and adverse effects.
While the researchers cannot exclude the possibility of a small benefit among children bathing more than five times a week or among children aged less than 5 years, they say differences are sufficiently small to be unlikely to be clinically useful.
As such, they say this trial "found no evidence of clinical benefit from including emollient bath additives in the standard management of eczema in children."
In a linked editorial, Carsten Flohr, Consultant Dermatologist from St John's Institute of Dermatology at Guy's & St Thomas' NHS Foundation Trust in London says: "Important remaining evidence gaps are optimal regimen for leave-on treatments, soap substitutes, and frequency of bathing in children with eczema."
So there is still some room for further work, "but it is heartening to see that an important evidence gap has been closed," he concludes. Both the NHS and families of children with eczema can now better invest in more effective treatments for this common and distressing condition.
More information: Emollient bath additives for the treatment of childhood eczema (BATHE): multicentre pragmatic parallel group randomised controlled trial of clinical and cost effectiveness, BMJ (2018). www.bmj.com/content/361/bmj.k1332
Editorial: New evidence challenges use of bath emollients for children with eczema, BMJ (2018). www.bmj.com/content/361/bmj.k1791


















