Accredited bariatric center reduces postop complications while increasing surgical volume
An academic medical center's weight-loss surgery program greatly lowered its rates of several postoperative complications, including rehospitalization in the first month, surgical site and urinary tract infections, and bleeding, despite almost doubling its surgical volume over five years. Results of this multiyear quality improvement project were presented today at the American College of Surgeons (ACS) 2018 Quality and Safety Conference.
This quality improvement project took place at California-based Stanford Bariatric, one of more than 800 centers in the country that have earned accreditation through the Metabolic Bariatric Surgery Accreditation and Quality Improvement Program (MBSAQIP). Maintaining this voluntary credential, awarded jointly by the ACS and the American Society for Metabolic and Bariatric Surgery (ASMBS) since 2012, requires accredited centers to perform an annual quality improvement project.
"MBSAQIP accreditation drives quality improvement," said principal investigator John Morton, MD, MPH, FACS, FASMBS, chief of bariatric and minimally invasive surgery, Stanford (Calif.) University School of Medicine. "Accreditation at hospitals performing bariatric surgery has been shown to decrease complications, costs, and deaths."
Stanford's bariatric surgery program identified complications needing improvement by reviewing the MBSAQIP Semiannual Report, which Dr. Morton likened to a report card. This risk-adjusted report contains participating centers' combined outcomes as well as center-specific data, explained Dr. Morton, who is the Chair of the Committee for Metabolic and Bariatric Surgery (CMBS), the surgeon oversight committee of MBSAQIP, Although MBSAQIP ranked Stanford as "exemplary" in most categories in 2013, "we wanted to do better. We wanted to provide the best care possible for patients."
The Stanford project committee chose reducing surgical site infections (SSIs) for their first improvement effort in 2013. They instituted "lean" methods of process improvement involving standardization and follow-up. Team members educated personnel in the operating room, emergency department, inpatient wards, and outpatient clinics about the improvement initiative. In monthly meetings, the entire bariatric program staff reviewed outcomes data, identified the root causes of SSIs that occurred, and discussed how to prevent these complications. In each of the four subsequent years, the committee followed the same processes for the other selected outcome measures: bleeding, medication reconciliation, unplanned readmissions in the first 30 days after discharge from the hospital, and urinary tract infections (UTIs).
Medication reconciliation involves comparing a patient's current medicines with new prescription orders and the patient's medical record to resolve discrepancies at transitions in care: hospital admission, transfer, discharge, and outpatient follow-up appointments. This process aims to decrease medication errors and overuse.
Medication reconciliation is important for bariatric surgical patients, who usually require multiple medicines to treat obesity-related illnesses, Dr. Morton said. Because substantial weight loss after a bariatric operation often improves or resolves co-existing illnesses such as Type 2 diabetes, high blood pressure, high cholesterol, and obstructive sleep apnea,1 patients may no longer need some of their medications.
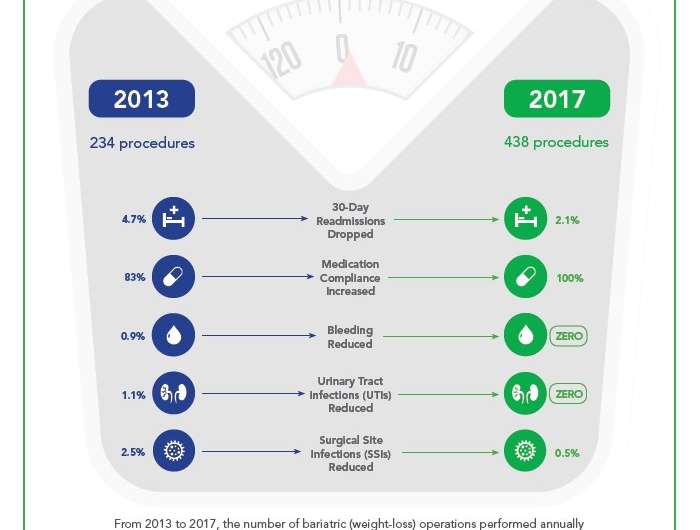
From 2013 to 2017, the number of bariatric operations performed annually at Stanford rose from 234 to 438, Dr. Morton reported. Yet, over the same five-year period, the bariatric surgery program reportedly saw the following improvements:
- 30-day readmissions: dropped from 4.7 percent to 2.1 percent of surgical cases
- Medication reconciliation compliance: increased from 83 percent to 100 percent of surgical cases
- Bleeding: decreased from 0.9 percent to zero
- UTIs: reduced from 1.1 percent to zero
- SSIs: reduced from 2.5 percent to 0.5 percent
To lower the readmission rate, the project team implemented a policy whereby nurses would contact each patient by phone after discharge. These phone calls allowed staff to identify problems and schedule follow-up appointments before a potential complication became severe enough to require rehospitalization.
The committee achieved full compliance with medication reconciliation, according to Dr. Morton, by requiring completion of that task in the patient's electronic health record before the health care provider could continue or close the record.
Bleeding is uncommon after bariatric surgical procedures, Dr. Morton said. However, it can occur where the surgeon attaches, often with staples, the newly reduced stomach pouch to the intestine. He said adding several sutures to the staple line helped lower the chance of bleeding in their patients.
Despite Stanford Bariatric's prior success in eliminating catheter-associated urinary tract infections (UTIs), they later encountered two patients with UTIs, Dr. Morton said. After investigation, the researchers discovered that UTIs were already present at admission in one-third of bariatric surgical patients. This finding, he said, led them to evaluate patients for potential UTIs preoperatively so that antibiotic therapy could begin when needed.
For reduction in SSIs, the committee initiated multiple evidence-based guidelines, including those from the ACS and the Surgical Infection Society.2 Among other efforts, the surgical team encouraged diabetic patients to have optimal preoperative blood glucose (sugar) control, which can affect wound healing; they asked patients to clean the surgical site at home before the operation; and they gave weight-based doses of antibiotics for infection prevention.
Dr. Morton concluded that the MBSAQIP Semiannual Report is an advantage to accreditation because it helps identify opportunities for improvement.
Another key to their successful quality improvement, he added, was persistence. He said, "It paid off—like putting money in the bank and getting interest."