Simple factors that can avoid harmful side effects in type 2 diabetes
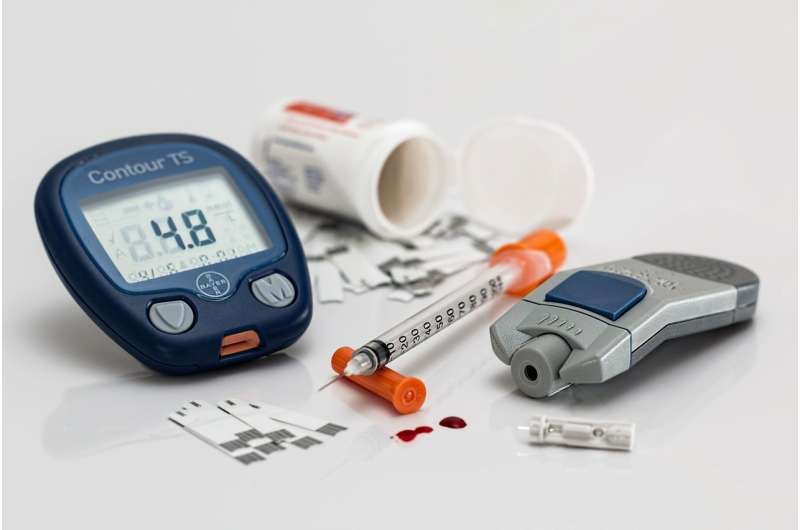
Clinicians can match people with type 2 diabetes to the right drug for them to improve control of blood sugar and help avoid damaging side-effects, simply by factoring in simple characteristics such as sex and BMI into prescribing decisions, new research has shown.
The study, by the University of Exeter Medical School, could dramatically improve benefits of drugs and reduce the risk of potentially harmful side-effects such as weight gain and hypoglycaemia, at no additional cost to the NHS.
Metformin is the first line of drug treatment in type 2 diabetes, but many patients will eventually need additional drugs on top of Metformin to lower their blood sugar levels. Currently, clinicians have to make prescribing decisions on these additional drug options based on limited available guidance. Recent research involving the Exeter team has revealed there is great regional variation across the UK in the prescribing of these additional drugs.
The new study, funded by the Medical Research Council and published in the journal Diabetes Care, provides a starting point for a more evidence-based approach to the prescribing of drugs after Metformin. Based on a patients' gender and BMI, the authors found important differences in the likely success of the commonly-prescribed drugs sulfonylureas and thiazolidinediones in lowering blood sugar levels, and in the risk of common side effects. For example, obese females were far more likely to have good blood glucose control on thiazolidinediones than sulfonylureas, whilst non-obese males had the opposite result—they were far more likely to have good blood glucose control on sulfonylureas than thiazolidinediones.
The Exeter team used anonymous data from more than 29,000 patients who had either taken part in trials or were treated in UK GP practices. By combining these datasets, the researchers were able to show their findings are robust and potentially applicable to many of the 3.5 million-plus people currently diagnosed with type 2 diabetes in the UK.
John Dennis, of the University of Exeter Medical School, was lead author on the study. He said "Our findings are important as they provide the first evidence that personalised or 'precision' medicine approaches in diabetes can be based on simple patient characteristics available to any doctor, rather than expensive genetics or other technology. This simple personalised approach could be implemented immediately within the NHS without any additional cost.
The study is also a powerful demonstration of how the sharing of patient data can meaningfully benefit patients—in this case helping to make sure individual patients get the best drug for them."
Professor Andrew Hattersley, a Consultant in Diabetes at the Royal Devon and Exeter Hospital and Research Professor at the University of Exeter Medical School said: "At the moment, clinicians are in the difficult position of making decisions that impact on health in type 2 diabetes based on very little evidence. Now, we can create clear guidelines to enable much more informed conversations about what these treatments will mean for people, in order to get better health outcomes and avoid harmful side effects."
Dr. Richard Evans, Programme Manager for Stratified Medicine and Molecular Pathology at the MRC, said: "This research used shared clinical trial data from a large number of patients to show that simple patient characteristics can help inform the choice of therapy in diabetes; the results are likely to show real impact, and significant benefits to patients when they are implemented in patient care.
"Diabetes afflicts one in 17 people in the UK—research into precision or stratified approaches to this condition is crucial to getting patients the most appropriate treatment in the most efficient way, underpinned by solid evidence."
The full paper, 'Sex and BMI alter the benefits and risks of sulfonylureas and thiazolidinediones in type 2 diabetes: A framework for evaluating stratification using routine clinical and individual trial data', is published in Diabetes Care.