Urgent care visits increase as emergency room visits fall
Treatment for new health problems, or acute care visits, encompass over one-third of all ambulatory care delivered in the United States. Given the high costs of emergency departments, many insurance plans have created incentives to encourage patients to receive that care elsewhere. In response to patient expectations for more convenience and to long wait times at traditional physician outpatient practices, alternative care facilities such as urgent care centers, retail clinics, and telemedicine have rapidly emerged.
In a study published today in JAMA Internal Medicine, Brigham and Women's Hospital researchers document that among private health plan enrollees, in recent years, there has been a substantial shift from emergency departments to urgent care centers when it comes to patients receiving care for low-acuity conditions.
"The drop-in emergency department visits are quite striking and represent a substantial shift in where patients go to get care for conditions such as sore throat and minor injuries," said Sabrina Poon, MD, MPH, who was an emergency physician and research fellow at BWH when the research was conducted.
In the cohort study, a team of investigators focused on the period between January 2008 and December 2015, examining de-identified data from Aetna, a large, commercial health insurance company, which insured approximately 20 million members per study year.
The team found that from 2008 to 2015 there was a large drop in emergency room visits and a substantial increase in the use of urgent care centers. Retail clinics and telemedicine utilization also increased substantially during this time, but when compared to urgent care centers and emergency rooms, they still accounted for a small number of visits.
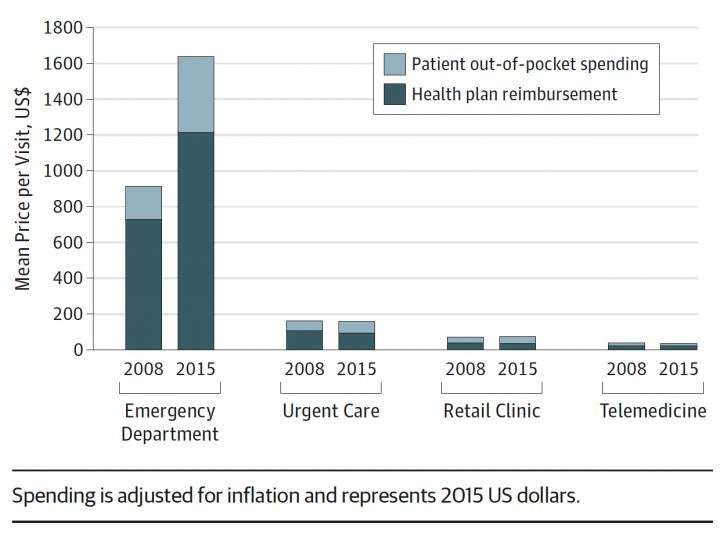
Visits to the emergency room for the treatment of these low-acuity conditions decreased by 36 percent, whereas use of non-emergency room centers increased by 140 percent. There was an increase in visits to all other venues, including a 119 percent increase at urgent care centers. Overall, across all acute care centers, the number of visits increased by 31 percent and spending associated with low-acuity conditions increased by 14 percent. The increase in spending was primarily driven by a 79 percent increase in price per emergency room visit for treatment of low-acuity conditions.
The researchers hypothesize that the reason for this growth is due to the increasing number of urgent care clinics, the familiarity and acceptance of urgent care centers as credible alternative venues among the community, their ability to treat a wide range of conditions, their convenience factor, shorter wait times, and lower out-of-pocket costs. Additionally, the investigators also found that among the population of patients with commercial insurance, patients with higher incomes were more likely to use non-emergency room clinics compared to people with lower incomes. Factors such as transportation and availability of alternative options may influence this care pattern.
These findings suggest that while the overall use of acute care venues for treatment of low-acuity conditions—and the associated spending—continue to rise, it is shifting from emergency rooms to urgent care centers.
"The increasing popularity of alternatives to the emergency department is likely being driven by a variety of factors, including cost, convenience, and long wait times," said Jay Schuur, MD, MHS, emergency physician at BWH and an author on the paper. "The overall increase in spending was driven by a 79 percent increase in price per emergency department visit as shown in the Table. In the next few years, it will be important to see how these trends evolve and whether the growth of alternative sites results in lower cost care or more use of medical care."
More information: Poon SJ, Schuur JD, Mehrotra A. Trends in Visits to Acute Care Venues for Treatment of Low-Acuity Conditions in the United States From 2008 to 2015. JAMA Internal Medicine (2018). DOI: 10.1001/jamainternmed.2018.3205