Study reveals that cells involved in allergies also play a key role in survival
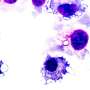
In a University of California, Irvine-led study, researchers found evidence that mast cells, an important group of immune cells typically associated with allergies, actually enable the body to survive fasting or intense exercise. The study was published today in Cell Metabolism.
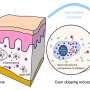
Typically found in the lungs and nose, mast cells are best known for their role in the body's allergic response. During an allergy attack, mast cells release a chemical called histamine into the bloodstream, which causes sneezing, runny nose, and other symptoms related to allergies. Drugs used to treat allergies block the annoying consequences of mast cell activity.
In this new study, led by Daniele Piomelli, Ph.D., professor of anatomy and neurobiology at UCI School of Medicine, and director of the UCI Center for the Study of Cannabis, researchers found that fasting causes the release of histamine from a select group of mast cells present in the gut, not those in the lungs or the nose. The histamine released from the gut travels to the liver where it triggers the formation of a fat-derived molecule called oleoylethanolamide (OEA).
Until now, researchers thought that OEA's main role was to block hunger. This new study indicates that histamine-triggered OEA formation in the liver stimulates ketogenesis, the conversion of fatty acids released from fat stores into chemicals called ketone bodies. Ketone bodies are vital to survival, because they keep the brain and muscles active during a prolonged fast or intense physical exercise.
"Without mast cells, histamine or OEA, we could not survive a marathon or a day-long hike without snacks, or any long period of time without food," said Piomelli. "What's fascinating to me is that a cell that was supposed to be the 'bad guy' in allergies, is the same one that allows us to survive prolonged lack of food or major physical effort."
Further research will be needed to determine if diseases that affect the ability of mast cells to release histamine and trigger OEA production could lead to disorders like liver steatosis, a precursor for liver fibrosis and cancer.