Diabetes drug impacts gut microbiome

Acarbose, a drug commonly used to treat type II diabetes, can change the gut microbiome in a reversible and diet-dependent manner, according to new research published in the journal mSphere. The findings highlight the importance of the gut microbiome in health and show that more attention should be paid to how the gut microbiome responds to medications.
"Acarbose has the potential to change the gut microbiome, but it is a very diet- dependent change," said study principal investigator Nicole Koropatkin, Ph.D., Assistant Professor of Microbiology and Immunology, University of Michigan Medical School, Ann Arbor, Michigan. "With medications, especially those that affect diabetes, we have to think about not only the impact the drug has on host enzymes or host metabolism, but how it affects gut bacterial metabolism. We know that there seem to be certain gut bacteria compositions that are more closely linked with diabetes and that might even precede the clinical onset of diabetes."
In recent years, researchers have learned that the gut microbiome of people with diabetes and otherwise healthy individuals differ. Scientists have also learned that the popular diabetes medication metformin exerts its medicinal effect, in part, by changing the gut microbiota in a manner that improves glucose tolerance. This is in addition to metformin impacting host glucose metabolism.
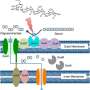
In her work as a protein crystallographer studying starch-degrading enzymes, Dr. Koropatkin became interested in acarbose, and set out to determine whether this diabetes drug might also spark off-target effects on the microbiota that might affect the drug's therapeutic benefits. Acarbose inhibits glucoamylase enzymes in the small intestine to prevent dietary starch digestion and thus decrease postprandial blood glucose levels. This results in an increase in dietary starch to the distal intestine where it becomes food for the gut bacterial community.
To investigate, Dr. Koropatkin teamed up with Dr. Patrick Schloss, Professor of Microbiology and Immunology at the University of Michigan Medical School, who focuses on host-microbiome interactions. They examined the effect of acarbose therapy, both a low dose and a high dose, on the gut community structure in mice fed either a high starch or high fiber diet rich in plant polysaccharides. "We wanted to try as much as we could to mimic the way that acarbose is administered to humans," said Dr. Koropatkin. "When humans start taking acarbose therapy, they usually start on a low dose, and then they move to a higher therapeutic dose."
The researchers found that the fecal microbiota of animals consuming a low dose of acarbose (25 ppm) was not significantly different from control animals that did not receive acarbose. However, feeding a high dose of acarbose (400 ppm) with a high starch diet substantial changed the gut microbiota structure. Short chain fatty acids measured from stool samples increased, especially butyrate, as a result of acarbose treatment in both diets. Most notably, said the researchers, the high starch diet with a high dose of acarbose lead to an expansion of the Bacteroidaceae and Bifidobacteriaceae and a decrease in the Verruocomicorbiacea and the Bacteroidales S24-7. Once the treatment stopped, the gut composition quickly reverted to mirror the control group, suggesting that the drug does not permanently impact the gut community. The high dose of acarbose in the plant polysaccharide diet resulted in a distinct community structure with increased representation of Bifiidobacteriaceae and Lachnospiraceae.
"Our study shows that acarbose feeding changes the gut community structure in a reversible and diet-dependent manner, which may have implications for how these medications are ideally administered in humans," said Dr. Koropatkin.
At present, Dr. Koropatkin said a high fiber diet is still the best recommendation for an individual with diabetes or a healthy person. "From everything we know about the gut microbiota, the best thing to do is eat a high fiber diet," said Dr. Koropatkin. "This is your best chance for keeping and collecting a microbiome that produces a lot of short chain fatty acids that regulate immune development and energy homeostasis."
Dr. Koropatkin said the short chain fatty acid butyrate, in particular, has received a lot of attention because it has anti-inflammatory and anti-tumorogenic effects. "Any therapy that could potentially increase butyrate production is worth considering when we think about ways to curb intestinal and systemic inflammation," said Dr. Koropatkin.