Collaboration sees sustained increase in imaging history quality from ordering providers
According to an ahead-of-print "Focus On" article published in the November issue of the American Journal of Roentgenology (AJR), collaborative research has not only standardized the definition of a complete imaging history, but also engineered systems to include supportive prompts in the order entry interface with a single keystroke—sustainably improving the quality of imaging histories, themselves.
A Kaiser Permanente multidisciplinary team—physicians, both primary care and medical imaging providers, as well as information technology and practice improvement professionals—first defined the various components of a complete imaging history, a process that underwent several improvement cycles where consensus audits were regularly performed.
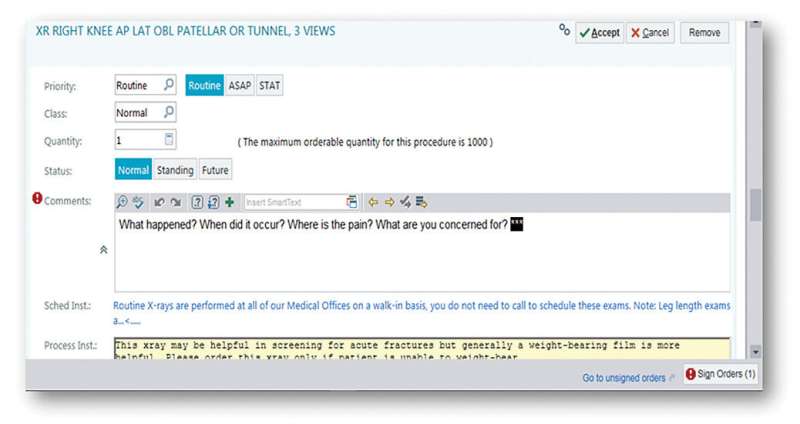
The final apparatus of the collaborative team's complete imaging history definition included the following responses:
- what happened;
- when it happened;
- where the patient was experiencing pain;
- and the ordering provider's concern.
These four prompts were then inserted into the electronic physician order entry process, and performance was monitored for an additional 18 months.
From March 13, 2017 to December 16, 2018, 10,236 total orders were placed by ordering providers in the study clinic. Of the orders audited in the baseline period, 16.0% (64/397) contained all four history components, which increased to 52.0% (2200/4234; absolute increase of 36.0%, relative increase of 225.0%; p < 0.0001) in the subsequent time periods.
Moreover, the mean number of characters ordering providers entered into the imaging histories they submitted increased from 45.4 characters per order during the baseline period to 75.4 (66.1% increase, p < 0.0001) after the intervention.
"Before this intervention, ordering providers in the institution were provided a single free-text box to enter whatever history information they felt to be relevant," wrote Daniel S. Bor from Kaiser Permanente's Department of Medical Imaging. "Our medical imaging team identified that frequently these unguided histories were incomplete, inconsistent, and of variable quality."
"Anecdotally," Bor continued, "radiologists have attributed the ability to make difficult diagnoses, such as subtle stress fractures, to having access to more complete imaging histories from ordering providers. We have also noticed that increased clinical information results in radiologists feeling less of a need to recommend additional downstream or repeat imaging."
Bor noted, too, that the project team remains optimistic that the emergence of artificial intelligence could facilitate an automated method to improve imaging histories and support high-quality radiologist interpretations.
More information: Daniel S. Bor et al, Sustained Increases in the Quality of Imaging Histories Provided by Ordering Providers Resulting From Multidisciplinary Collaboration and Systems Design, American Journal of Roentgenology (2019). DOI: 10.2214/AJR.19.21513