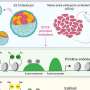
Outcomes of birth options after a previous cesarean section

A large cohort study of women who have had one or more previous cesarean sections suggests that attempting a vaginal birth in a subsequent pregnancy is associated with higher health risks to both the mother and the infant than electing for another cesarean.
The research, published in the open access journal PLOS Medicine on September 24, addresses a lack of robust information on the outcomes of birth options after previous cesarean section and can be used to counsel women about their choices.
Around the world there have been increases in cesarean section deliveries, leading to a larger proportion of pregnant women with a history of cesarean section. Guidelines recommend that these women be counselled about the benefits and harms of planning a subsequent cesarean or attempting a vaginal birth yet there is little evidence around this.
Kathryn Fitzpatrick of the Nuffield Department of Population Health, University of Oxford, and colleagues used data from 74,043 full term births of single babies in Scotland between 2002 and 2015. For women who have had previous cesarean section, the researchers estimated the short term maternal and perinatal health outcomes associated with attempting a vaginal birth compared to planning another cesarean section. 45,579 women gave birth by planned cesarean and 28,464 attempted vaginal birth, 28.4% of whom went on to have an emergency cesarean section.
Attempting vaginal birth was associated with an increased risk of the mother having serious birth and post-birth related problems compared to electing for another cesarean section. Attempting vaginal birth was more likely to result in uterine rupture (69 vs 17 women, adjusted odds ratio [aOR] 7.3, 95% confidence interval [CI] 3.9-13.9), a blood transfusion (324 vs 226 women, aOR 2.3, 95% CI 1.9-2.8), sepsis (76 vs 78 women, aOR 1.8, 95% CI 1.3-2.7 ), surgical injury (aOR 3.0, 95% CI 1.8-4.8), and more serious infant outcomes such as stillbirth, admission to neonatal unit, resuscitation requiring drugs or intubation, or an Apgar score less than seven at five minutes (2,049 vs 2,570).
It should be noted that the absolute risk of complications were small for either type of delivery. Overall, just 1.8% of those attempting a vaginal birth and 0.8% of those having a planned cesarean experienced serious maternal complications. 8.0% of those attempting a vaginal birth and 6.4% of those having a planned cesarean had one or more of the adverse infant outcomes examined.
Kathryn Fitzpatrick, who led the study, said: "Our findings can be used to counsel and manage women with previous cesarean section and should be considered alongside existing evidence on the increased risk of serious maternal morbidity in subsequent pregnancies associated with elective repeat cesarean section." Further studies are needed to confirm these findings and investigate the longer-term outcomes associated with multiple cesareans or attempting vaginal birth following previous cesarean.
More information: Kathryn E. Fitzpatrick et al, Planned mode of delivery after previous cesarean section and short-term maternal and perinatal outcomes: A population-based record linkage cohort study in Scotland, PLOS Medicine (2019). DOI: 10.1371/journal.pmed.1002913