How Crohn's disease-associated bacteria tolerate antibiotics
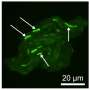
Bacteria associated with Crohn's disease rely on multiple stress responses to survive, multiply, and tolerate antibiotics within white blood cells called macrophages, according to a study published November 14 in the open-access journal PLOS Pathogens by Olivier Espéli of the College de France and PSL Research University in Paris, France, and colleagues.
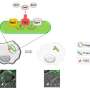
Crohn's disease is a chronic disease that causes inflammation and irritation in the digestive tract. The disease is characterized by an imbalance in the intestinal microbiome. In particular, adherent-invasive Escherichia coli (AIEC) strains have been implicated in the disease. AIEC colonize intestinal cells and survive and replicate within macrophages. In the new study, the researchers demonstrated that the AIEC LF82 strain can switch between replicating and non-growing states within macrophages. This switch can result from a stress response called the stringent response immediately after uptake by macrophages, or at later stages, from DNA damage and a stress response called SOS during replication within macrophages.
First, a stress response called the stringent response halts the replicative cell cycle of AIEC LF82 for a few hours, during which a large number of AIEC LF82 acquire the ability to tolerate antibiotic treatments. Later, when AIEC multiplication restarts, it requires DNA repair, suggesting that AIEC have accumulated DNA damage during the first hours after infection. In this second phase, non-growing bacteria appeared frequently from the population of growing AIEC LF82, raising the proportion of antibiotic-tolerant AIEC LF82 by up to 10% of the population. The results suggest that a reservoir of antibiotic-tolerant, non-growing bacteria could be responsible for long-term survival in the host as well as relapsing infections.
Espéli adds, "Within their macrophage's niche, Crohn's disease associated bacteria become tolerant to antibiotics."
More information: Gaëlle Demarre et al, The Crohn's disease-associated Escherichia coli strain LF82 relies on SOS and stringent responses to survive, multiply and tolerate antibiotics within macrophages, PLOS Pathogens (2019). DOI: 10.1371/journal.ppat.1008123