What interventional radiologists need to know about frostbite and amputation
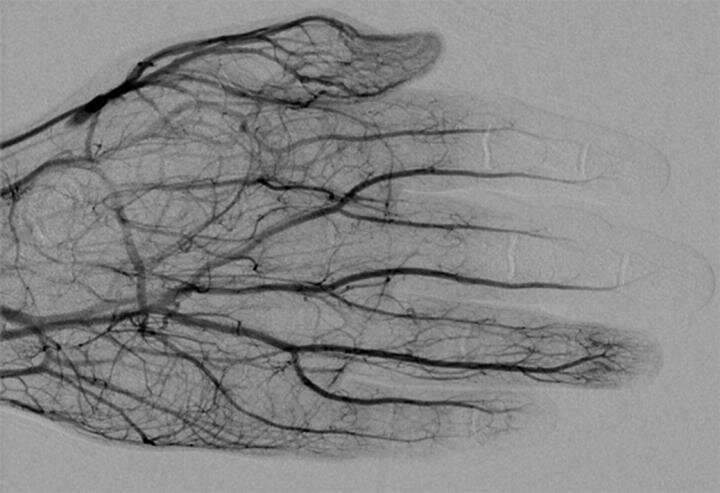
An ahead-of-print article in the April issue of the American Journal of Roentgenology (AJR) reviewing various techniques and clinical management paradigms to treat severe frostbite injuries—relevant for interventional radiologists, especially—showed promising results using both intraarterial (IA) and IV tPA (tissue plasminogen activator) to reduce amputation.
"Severe frostbite injuries can lead to devastating outcomes with loss of limbs and digits, yet clinical management continues to consist primarily of tissue rewarming, prolonged watchful waiting, and often delayed amputation," wrote Boston Medical Center radiologists John Lee and Mikhail Higgins.
A search of the literature by Lee and Higgins yielded 157 citations. After manually screening for inclusion criteria of case reports, case series, cohort studies, and randomized prospective studies that reported the use of tPA to treat severe frostbite injuries, 16 qualified for review.
Lee and Higgins' analyzed series included 209 patients with 1109 digits at risk of amputation treated with IA or IV tPA—116 and 77 patients, respectively. A total 926 at-risk digits were treated with IA tPA and resulted in amputation of 222 digits, for a salvage rate of 76%. Twenty-four of 63 patients underwent amputation after IV tPA, resulting in a 62% salvage rate.
Both digital subtraction angiography (DSA) and triple-phase bone scan were utilized for initial imaging evaluation of patients with severe frostbite injuries.
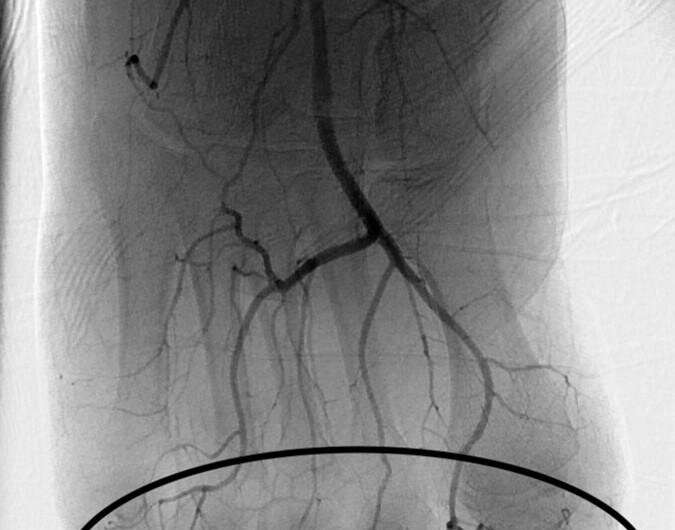
Additional concurrent treatment included therapeutic heparin at 500 U/h, warfarin with target international normalized ratio of 2:3, nonsteroidal anti-inflammatory drugs, pain management, and light dressings with topical antimicrobial agents.
"For many years," Lee and Higgins concluded, "the axiom 'frostbite in January, amputate in July' was an accurate description of the common outcome in frostbite injuries. Through a meta-analysis of thrombolytic therapy in the management of severe frostbite, this article provides a useful guideline for interventional radiologists, including a suggested protocol, inclusion and exclusion criteria, and potential complications."
More information: John Lee et al, What Interventional Radiologists Need to Know About Managing Severe Frostbite: A Meta-Analysis of Thrombolytic Therapy, American Journal of Roentgenology (2020). DOI: 10.2214/AJR.19.21592


















