Loss of 'Jedi' receptor alters neuron activity
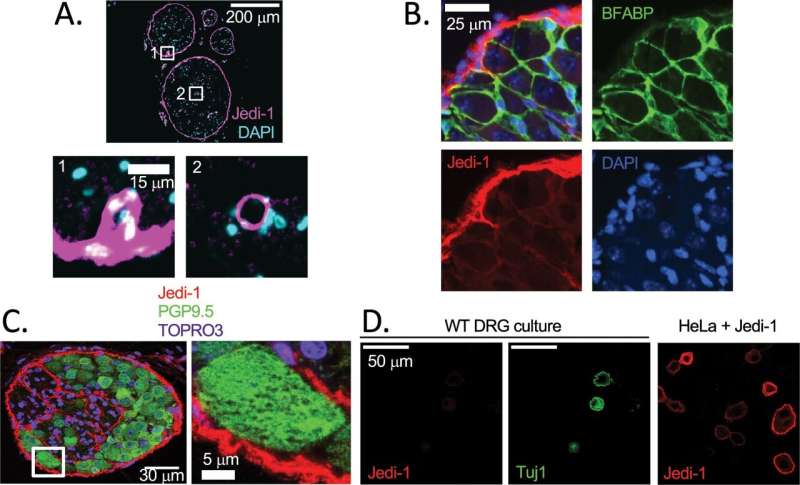
The cell bodies of peripheral sensory neurons that respond to and transmit information about stimuli including touch, temperature and pain reside in the dorsal root ganglia (DRG). DRG neuron hyperexcitability is correlated with chronic pain.
Bruce Carter's group previously identified Jedi-1, a receptor expressed by satellite glia in the DRG that plays a role in the normal clearance of DRG neurons that die during development.
Graduate student Alexandra Trevisan and colleagues further investigated Jedi-1 function in vivo using mice lacking Jedi-1. They were surprised to find changes in DRG neuron activity, despite the fact that sensory neurons do not express Jedi-1. They demonstrated an increase in the fraction of capsaicin-sensitive neurons, increased excitability, altered firing patterns and changes in sodium currents.
The study in Scientific Reports shows that loss of Jedi-1 alters DRG neuron activity indirectly through an interaction between non-neuronal cells and sensory neurons. Targeting neurons through glial cells may be an alternative treatment for chronic pain, the authors suggest.
More information: Alexandra J. Trevisan et al. Jedi-1 deficiency increases sensory neuron excitability through a non-cell autonomous mechanism, Scientific Reports (2020). DOI: 10.1038/s41598-020-57971-2