Partial measures compromise effectiveness of efforts to combat COVID-19
Comprehensive implementation of COVID-19 infection prevention measures boosts their effectiveness, while partial implementation compromises it. These are the findings from a study led by Prof. Setsuya Kurahashi at the Faculty of Business Sciences, University of Tsukuba.
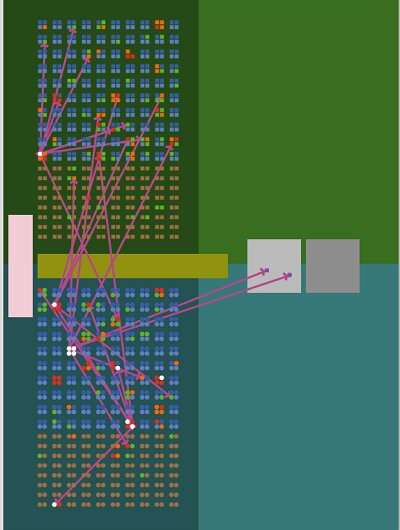
The team developed an agent-based computer model to estimate the effects of staggered commuting times, telecommuting, school closures, social distancing, self-isolation, and the various other measures being used in an effort to halt the spread of COVID-19, the novel coronavirus. Simulations conducted using this model showed that implementing measures either individually or in partial combinations yields limited results. The findings provide hints for estimating the combinations of measures most effective in preventing the spread of infection.
As governments, local authorities, research institutions, and the media all present a multitude of measures to combat the spread of COVID-19 such as washing and disinfecting hands, wearing masks, avoiding the "three Cs" (closed spaces, crowded places, close-contact settings), self-isolating, telecommuting, staggered commuting times, videoconferencing, and school closures, the lack of hard data makes comprehensive estimation of effectiveness difficult. This study seeks to fill that gap by modeling the COVID-19 infection process in a range of scenarios involving different behaviors.
The model compared the effectiveness of different measures against the COVID-19 infection process on the populations, workplaces, and schools of two virtual "towns." The residents were exposed to the risk of infection through commuting to work and school, and visiting shops and other everyday places. Hospitalizations, deaths, and infection speeds were simulated across 27 combinations of preventive measures, including no measures at all, basic measures only, combinations of basic measures, and combining basic measures with reduced contact with other people.
Combinations that incorporated telecommuting, school closures, and stay-home measures suggested the greatest efficacy, while measures implemented alone or in partial combinations did not result in any drop in hospitalization numbers, and were not effective as infection prevention measures. Moreover, in all of the permutations covered, elderly people made up a far greater proportion of those hospitalized and critically ill, thus indicating that preventing infection among the elderly may lead to fewer hospitalizations and deaths overall. However, any chink in the armor was enough to compromise effectiveness in these models, and the risk of infection remained high.
In addition, the model used in this study has already provided insights regarding other factors in the spread of COVID-19, including the effects of events where crowds gather (conclusion: the type of event has a greater effect than the scale), the effects of increased PCR testing (more testing of those who may be infected may help inhibit infection), and the effects of lockdowns and their durations (late and incomplete lockdowns resulted in recurrences of COVID-19).
The team is hopeful that these studies will help speed up the discovery of the most effective measures for combatting COVID-19.
More information: Setsuya Kurahashi. Estimating Effectiveness of Preventing Measures for 2019 Novel Coronavirus Diseases (COVID-19), Transactions of the Japanese Society for Artificial Intelligence (2020). DOI: 10.1527/tjsai.D-K28