Researchers succeed with a more inclusive approach to heart transplants
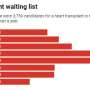
Doctors at Yale New Haven Hospital used a more aggressive selection process to more than quadruple the number of heart transplants performed there while maintaining positive patient outcomes, according to a new study.
The findings suggest that a more inclusive approach to selecting donor hearts and transplant recipients can enable hospitals to successfully treat more patients in need of transplants. The study appears online Sept. 18 in the journal JAMA Network Open.
The study looked at short-term patient outcomes for two groups: 49 patients who received heart transplants from 2014 to 2018, and 58 patients who had their heart transplants in the year after the hospital adopted a more aggressive selection process for donor recipients (2018-2019).
The more aggressive selection process significantly shortened the waiting period for heart patients, from 242 days to 41 days, the researchers said. Importantly, patients' survival rate at 180 days after the transplant remained nearly unchanged.
The expansion of heart transplant procedures at the hospital, in September 2018, coincided with the implementation of the new United Network for Organ Sharing (UNOS) donor heart allocation system in the United States.
"I think this is the takeaway for other centers—that such a change in the approach could create opportunities for patients in need while maintaining outcomes in the short term," said Makoto Mori, M.D., a surgical resident at Yale and first author of the study.
The senior author of the study was Harlan Krumholz, M.D., the Harold H. Hines Jr. Professor of Medicine (cardiology) and director of Yale's Center for Outcomes Research and Evaluation.
In practical terms, the expansion of heart transplant procedures at Yale New Haven Hospital meant accepting hearts from older donors with additional medical conditions, as well as accepting transplant recipients with more severe illnesses.
Yale New Haven Hospital also changed the surgical leadership of its advanced heart failure program, hired a dedicated procurement surgeon and an additional transplant coordinator, and increased the involvement of surgical attending physicians.
The researchers noted that Yale's increase in heart transplant cases was significantly larger than the volume change seen at other heart transplant centers in the same region during the same period, including Hartford Hospital, Tufts Medical Center, Brigham and Women's Hospital, and Massachusetts General Hospital.
"We used a multidisciplinary approach and made strategic changes in donor and recipient selection, which allowed us to increase the number of heart transplants performed and therefore help more patients with advanced heart failure in a safe and an effective manner," said co-author Arnar Geirsson, M.D., chief of cardiac surgery at Yale New Haven Hospital.
Co-authors of the study were Lynn Wilson, Tariq Ahmad, Muhammad Anwer, and Daniel Jacoby, all of Yale; and Ayyaz Ali of Hartford Hospital.