Clinical study aims to better understand COVID-19 immunity
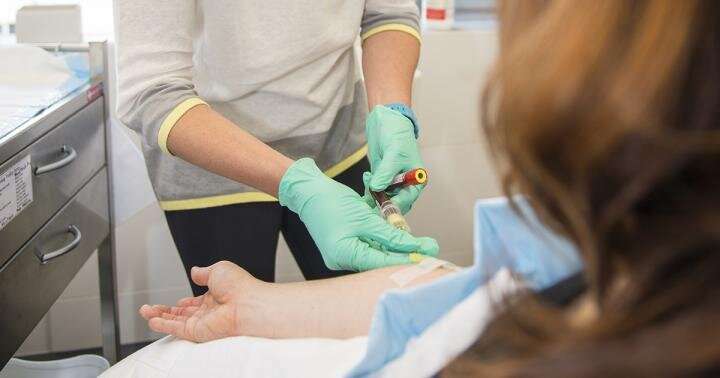
People who have recovered from COVID-19, and their close contacts, could hold the key to understanding how immunity to the disease develops, how long it lasts and what happens when immunity is lost.
The COVID PROFILE study, led by the Walter and Eliza Hall Institute, will use blood samples from people in Victoria to look in detail at immune responses to COVID-19, to reveal how people are protected—and how long people are protected—from future COVID-19 infection. This information is vital for vaccine development—and could explain whether future vaccines can be given once, or whether they will need to be regularly repeated, like the annual influenza vaccine. This information will be critical for planning for the long-term 'COVID-normal' both locally and internationally.
At a glance
- Melbourne researchers are investigating the immunity effects of COVID-19
- The study is recruiting people who have had COVID-19 and their close contacts who haven't contracted the virus
- The research will help inform decisions about vaccine development and other public health measures to control the virus, including operating in a 'COVID-normal' society
Understanding immunity against COVID-19
The study is looking for 300 adult volunteers, both those who have had COVID-19 and those who were close contacts (such as household members) but did not contract the disease. These participants will be followed for 12 months after their exposure to COVID-19, through regular blood samples and nose and throat swabs.
Lead researcher Professor Ivo Mueller said there were big questions in the scientific community about whether people could be re-infected with COVID-19 or how long immunity offered protection against the virus.
"While we know their immune response protects people after they recover from COVID-19, we suspect this protection wanes over time and reinfection of COVID-19 may be possible. We don't know how long this immunity lasts and whether it differs between people who have had severe, mild or asymptomatic infections," he said.
"Understanding immunity to COVID-19 is vital for developing vaccination strategies. It will also drive greater awareness and understanding to help us better manage this virus in the community.
"If we can predict the way immunity to the virus develops over time, whether and when people can be reinfected, and whether symptoms are less severe upon reinfection, we will be able to plan accordingly and stay ahead of the virus," he said.
Explaining different disease outcomes
As researchers across the world race to make sense of this global pandemic, many vital factors remain unknown.
"Concerningly, it may be possible that a second COVID-19 infection could be worse than the first, if immunity has waned. Our study will look closely at whether people could have more severe symptoms if they are re-infected," Professor Mueller said.
Study investigator Dr. Vanessa Bryant said the research was crucial in helping to understand the wide range of symptoms experienced by people with COVID-19.
"Some people get severely ill and require hospitalisation, while others are almost completely asymptomatic. Understanding why this happens will help us identify 'biomarkers' that could be used to predict which people may be at higher risk of contracting the virus or developing the most severe symptoms," she said.
"This will enable us to find new treatments that can help strengthen patients' immune systems to help them recover faster."