Study yields recommendations to prevent outbreaks from waterborne coronaviruses

Testing has shown that sewage systems can be flush with coronaviruses, and airborne coronaviruses traced to wastewater have been identified as the cause of at least one major disease outbreak. NC State University researchers are outlining strategies aimed at preventing similar outbreaks from happening again.
"We know that untreated water and wastewater can carry coronaviruses, and there is good evidence that wastewater previously led to coronavirus outbreaks. This suggests that something similar could happen with COVID-19," said Steven G. Hall, a biological engineer and one of the study authors. "The good news is you can do something about it—we found several effective control techniques—and one of the cheapest, simplest ways is chlorination, which is widely available and fairly easy to safely use.
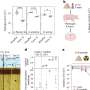
In an article appearing recently in the Nature research journal npj Clean Water, Diplina Paul, Praveen Kolar and Hall, of NC State's Department of Biological and Agricultural Engineering, summarize research into how waterborne coronaviruses can be inactivated. They also outline a multipronged approach for using that knowledge to limit or prevent waterborne transmission of the viruses.
The researchers draw their conclusions from a review of close to 100 articles in peer-reviewed journals focused on medicine, engineering, microbiology and other disciplines.
Could It Happen With COVID-19?
Paul, a Ph.D. student and the paper's lead author, says that while COVID-19 spreads predominantly by respiratory droplets, the fact that the virus that causes the disease is present in fecal and anal swabs of infected patients raises questions about whether it can be spread the way that the SARS coronavirus did in a Hong Kong apartment complex in 2003. During that outbreak, high concentrations of airborne viruses in building plumbing were drawn into apartment bathrooms through floor drains. More than 300 people were infected.
"In terms of structure, these viruses are quite similar—70 to 80%," Paul says. "So if SARS 2003 could lead to such cases, even the severe acute respiratory syndrome-virus we are dealing with now could lead to similar cases, especially if aerosolization can take place—and more so when plumbing has small holes or leaks that lead to the atomization of the wastewater."
When it comes to the persistence and survival of coronaviruses in water, temperature is the most important factor, Paul says, with high temperatures rapidly inactivating them. The presence of antagonistic microorganisms is also helpful, as are disinfectants such as chlorine and ultraviolet light.
On the other hand, high concentrations of organic matter favor the viruses' persistence, because the organic matter can absorb them and protect them from damaging light, disinfectants and other antiviral agents.
Researchers Recommend Updates and New Technology
Based on her study, Paul encourages hospitals and public clinics to update their wastewater treatment systems to reduce the aerosolization of virus-infected wastewater and to use decentralized wastewater treatment systems so that viruses aren't transmitted to the larger community.
She also suggests that in places in the world where sanitation facilities are limited, lime-treated pit latrines and public health and extension efforts could decrease the risks posed when human feces are disposed of in open spaces like fields, forests, beaches and waters.
The researchers also recommend the development of new sensing technologies that can be linked to alarms that would alert wastewater treatment plant workers to the presence of coronaviruses, allowing them to intervene rapidly to contain their spread. Kolar says that existing technologies could be combined to create such a system.
In addition, Kolar stresses the potential for UV-based portable devices for wastewater treatment and centralized community drinking water treatment to provide water that is free of coronaviruses.
The authors conclude that "apart from adhering to the three vital Ws: washing hands often, wearing a nose and mouth covering to restrict aerosolization of droplets, and waiting 6 feet apart from others, adequate disinfection of potentially virus-laden water and wastewater with best management practices would help us to control … future waterborne outbreaks."
More information: Diplina Paul et al. A review of the impact of environmental factors on the fate and transport of coronaviruses in aqueous environments, npj Clean Water (2021). DOI: 10.1038/s41545-020-00096-w