Improving patient outcomes with clearer health monitoring data
According to the Center for Disease Control and Prevention, heart disease and its effects are the leading cause of death in the U.S. across a majority of racial and ethnic groups. Globally, the risk factors for developing heart disease, such as obesity and diabetes have grown by huge margins, increasing the future impact of heart disease on society and medical infrastructures. As with many chronic or long-term health issues, the successful management of heart disease can greatly improve a patient's lifespan and quality.
This successful management requires the collection of large datasets of the electrical signal of a patient's heart gathered from long-term measurements using an electrocardiogram (ECG) device. In the past, ECG data was collected in controlled clinical settings. However the development of new electronic materials and internet-connected devices have allowed the ECG to become a portable, wearable and commercially available product. Although these products are a great benefit to the patient users, they are not without flaws. The everyday motions of a patient, from walking to brushing their teeth, can alter the ECG data. These false recordings, called motion artifacts (MAs), can make it difficult for clinicians to detect abnormal heart rhythms that may be the signal of the onset of a heart attack.
Corrective solutions to the issue of MAs have, thus far, been either expensive to implement, such as filtering software, or cause discomfort to the wearer, such as tighter strap attachments and stronger, skin irritating adhesives. The team of W. Hong Yeo, Associate Professor in the George W. Woodruff School of Mechanical Engineering & PI of the Yeo Group & Director of Center for HCIE, working with partners at the Korea Advanced Institute of Science and Technology and Emory University have designed a flexibly packaged wireless wearable ECG device using a new class of strain-isolating materials that reduces MAs, induced by movement in the skin/sensor contact area.
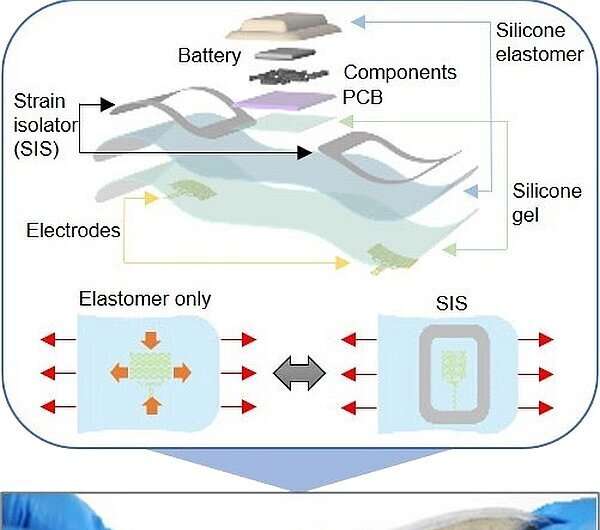
The team's new strain-isolated, wearable soft bioelectronic system (SIS) adheres naturally to the skin using a breathable soft membrane for continuous conformal contact. A pair of nanomembrane mesh electrodes and a thin-film circuit powered by rechargeable lithium-ion batteries are placed on a thin layer of silicone gel to allow a greater range of motion and packaged within a low modulus silicone elastomer. In testing the design against commercially available skin-mounted biosensors, the team's new device provides real-time wireless data of multiple physiological signals with a significant reduction in MA interference. Additionally, and most importantly, the device trial participants exhibited no device lamination issues, excessive sweating, signal degradation, or increased skin irritation.
Yeo and his team are pleased with their results to-date but have plans to take the research even further. The team seeks an even smaller device footprint by integrating fan-out wafer-level packaging and developing all-printing fabrication methods. Additionally, the team is planning large-scale clinical studies in cardiology and pediatrics to monitor the health status of both inpatient and outpatient groups on a continuous basis.
More information: Nathan Rodeheaver et al, Strain‐Isolating Materials and Interfacial Physics for Soft Wearable Bioelectronics and Wireless, Motion Artifact‐Controlled Health Monitoring, Advanced Functional Materials (2021). DOI: 10.1002/adfm.202104070