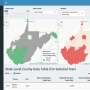
One way some drug prosecutions may be hurting public health

A recent analysis raises concerns that prosecutions under so-called "drug-induced homicide" (DIH) laws may be exacerbating public health problems. The work focused on one North Carolina county, but highlights the need for broader research into the effects of DIH laws in more than two dozen states.
Broadly speaking, DIH laws allow for the prosecution of drug distribution to someone who dies from an overdose as equivalent to homicide or manslaughter. In other words, if Person A sells drugs to Person B, and Person B overdoses, Person A could face the equivalent of a murder sentence.
The recent analysis, which is the first published analysis to draw on empirical data, suggests that DIH laws may be threatening public health in at least two ways.
To learn more, we spoke with Jennifer Carroll, corresponding author of "Drug induced homicide laws may worsen opioid related harms: An example from rural North Carolina," which was published in the International Journal of Drug Policy. Carroll is an assistant professor of medical anthropology at NC State and an adjunct assistant professor of medicine at Brown University. Carroll's collaborators were Bayla Ostrach of Boston University; Loftin Wilson, Reid Getty and Jesse Bennett of North Carolina Harm Reduction Coalition (NCHRC); and Jesse Lee Dunlap, formerly of NCHRC.
Question: To understand what's happening in this paper, you have to know a little about a particular drug-related conviction in Haywood County, North Carolina. What do folks need to know about the case?
Jennifer Carroll: In 2019, the North Carolina General Assembly passed the state's "Death by Distribution" law. The law allows for the prosecution of drug delivery resulting in a fatal overdose as equivalent to homicide. The law was inspired by a local case brought against a resident of Haywood County in 2017 in connection with the tragic and accidental overdose death of a young woman. The individual who supplied the drugs (an illicit opioid) that later contributed to the overdose death was charged with second-degree murder and, in 2018, was sentenced to more than 30 years in prison—a sentence more than three times longer than the maximum allowable prison sentence for selling drugs in North Carolina.
The case received an enormous amount of media attention—so much attention that it caught the interest of N.C. Rep. Dean Arp, who authored the Death by Distribution law with the assistance of the same district attorney who brought the murder case in Haywood County.
Question: How did you run across this case?
Jennifer Carroll: The person who was sentenced to several decades in prison for second-degree murder was well known in the local community. Haywood County is a small place, socially speaking, with only 60,000 or so residents. The community of people who use drugs in Haywood County is smaller still. It's a place where everybody knows everybody's business.
In the summer of 2019, I was in Haywood County conducting research in collaboration with the North Carolina Harm Reduction Coalition (NCHRC) – a non-profit organization that provides essential harm reduction services like access to sterile syringes and the overdose reversal medication naloxone. When we interviewed Haywood County residents who were utilizing these harm reduction services, we quickly found that they all had some kind of personal relationship to the defendant in the 2017 case. Some were acquaintances; some knew him very well. Talking about those relationships quickly revealed how much of an impact that case had on these residents. It weighed heavily on them emotionally, and they reported the case having real impacts on the local drug market and their individual risk factors for accidental overdose. It was those connections—the social-emotional impact and the public health consequences of the 2017 trial—that we wanted to explore.
Question: Why did you decide to do a separate analysis on DIH?
Jennifer Carroll: DIH laws (NC's Death by Distribution law is but one example) are increasingly common strategies for prosecuting drug distribution. According to data from Northeastern University's Health in Justice Action Lab, the number of charges brought under DIH laws in the United States has skyrocketed from two in the year 2000 to more than 700 in 2017—growth that has been in step with public attention on the opioid overdose epidemic.
There is significant, sometimes contentious, disagreement among researchers, legal scholars, and prosecuting attorneys in the state of North Carolina about whether bringing DIH charges is an appropriate moral or legal response to an accidental overdose death. There is greater disagreement about what impact such charges have on public health. Do these cases drive people who use drugs further underground and increase the likelihood of fatal overdoses by reducing people's willingness to call 911 in an emergency? Do these cases improve public health by taking dangerous actors off the streets or deterring the distribution of fentanyl through severe criminal punishments? Intelligent scholars and public servants have passionately levied both arguments. Yet, the reality is we simply don't know.
There is precious little research on trends in DIH charges. And there is no systematic research that we are aware of detailing how people who use drugs, including those most at risk of fatal overdose, are impacted. Even though we did not set out to study these cases, we realized we had obtained the first systematically-collected empirical evidence about the impact of DIH cases on local community members. We recognized the importance of placing this data in the scientific literature, so that others could have access to and learn from it.
Question: What did your analysis consist of?
Jennifer Carroll: I was conducting research with NCHRC to assess public health needs across the state. That involved a few weeks of interviewing local residents who use drugs and distributing surveys among harm reduction program participants. Separately, Dr. Ostrach was engaged in a long-term project exploring the implementation of evidence-based harm reduction strategies in Haywood County.
Question: Given the limited data set you had to work with, what were you able to conclude? And what were you able to infer?
Jennifer Carroll: Ultimately, we were able to develop a series of hypotheses, which accounted for individual behaviors, social proximity to the defendant in the 2017 case, and the passage of time since the defendant's 2018 sentencing, to explain how this DIH case impacted public health and the risk of opioid overdose in Haywood County. In sum, though the case could arguably be said to have produced some short-term reductions in opioid overdose risk, those positive benefits appear to be significantly outweighed by the negative, longer-term impacts of the case in the local community, including a more volatile drug supply and reduced willingness to call emergency services to the scene of an overdose.
While we can be confident that these impacts were felt by local residents of Haywood County, these hypotheses need to be tested and confirmed elsewhere.
Question: In the paper, you describe a couple ways that DIH prosecutions may be adversely impacting public health. Can you explain those?
Jennifer Carroll: Our data demonstrates a number of ripple effects in Haywood County stemming from this case. Local residents reported, in no uncertain terms, that the purity and potency of the local drug supply was significantly reduced soon after the trial. Specifically, they said that local drug suppliers were diluting their products to avoid the risk of overdose out of fear that they, too, could face murder charges. In the short term, that sounds like a positive public health impact from this case.
However, participants reported adjusting to this shift by buying and using larger quantities of drugs, making their regular habit more expensive and possibly leading them to inject drugs more often—increasing their risk of infection. The purity and potency of drugs then increased, returning to normal within a year of the sentencing. This could contribute to overdose among those who had a lowered opioid tolerance or who had started using more drugs at one time in response to the previously diluted drug supply.
Further, willingness to call 911 and seek emergency services during an overdose emergency plummeted following the 2018 sentencing. North Carolina has a 911 Good Samaritan Law designed to encourage calling 911 by extending limited immunity from criminal charges to someone who calls to request an ambulance during an overdose. Haywood County residents are well-educated about this law thanks to successful harm reduction education; therefore, outreach workers attributed this chilling effect to the high-profile sentencing of the local defendant. Finally, a blanket refusal to call 911 was more likely to be stated—and stated passionately—by people who were close members of the local defendant's social network.
Though not conclusive, our data suggests that this DIH case had a negative impact on public health and increased the risk of fatal opioid overdose for Haywood County residents.
Question: What do you think the big takeaway here is?
Jennifer Carroll: Our study demonstrates most conclusively that further research on the individual and community-level impacts of DIH laws is urgently needed.
More than 93,000 people—each of them someone's friend, child, or loved one—lost their lives to drug overdoses in 2020. Law-makers, prosecutors, and other public servants in the criminal-legal system are engaging the tools they have at their disposal in response to overwhelming loss in their communities. But with no science to guide these criminal-legal strategies, our public servants are flying blind.
Many prosecutors value DIH charges for the opportunities they represent to seek justice, support healing, and bring closure to families who have lost loved ones. But what if DIH prosecutions actually increase the chance that other families will suffer the same tragedy? We owe it to prosecutors and to our communities to produce reliable answers to that question.
More information: Jennifer J. Carroll et al, Drug induced homicide laws may worsen opioid related harms: An example from rural North Carolina, International Journal of Drug Policy (2021). DOI: 10.1016/j.drugpo.2021.103406