Health of some ethnic minority groups in the UK equivalent to White people at least 20 years older
A new study from researchers at the Universities of Sussex and Manchester, funded by the Nuffield Foundation, has revealed stark health inequalities between different ethnic groups that are influenced by persistent restrictions from life opportunities due to racism.
Inequalities in health becoming apparent from around age 30 and continuing to widen as people age, becoming particularly pronounced by the time that people are in later life, the study co-authored by Dr. Sarah Stopforth and Dr. Laia Becares at the University of Sussex reveals.
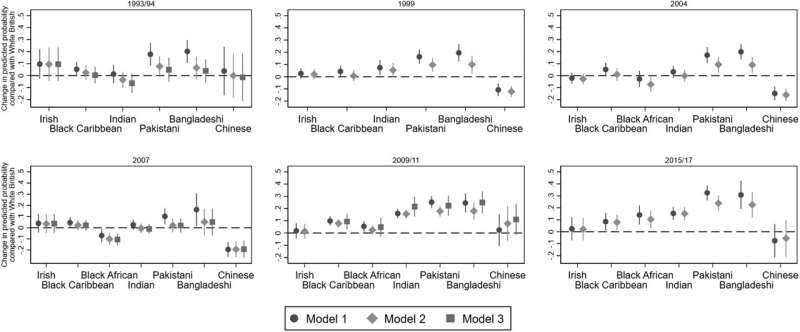
The research found that at any age after 30, people from Pakistani and Bangladeshi backgrounds experience the worst health of any ethnic group, with rates of poor health that are equivalent to those of White people at least 20 years older. For example, 22% of White British women in their 80s report poor health—the same proportion as for women from Pakistani backgrounds in their 50s (23%). And the rate of poor health for women from Bangladeshi backgrounds in their 40s (14%) is equivalent to that of White British women in their 70s (14%).
The analysis also shows that rates of poor health among men and women from Black Caribbean backgrounds are equivalent to those of White British people around ten years older. Overall, people from Pakistani backgrounds are twice as likely to report poor health than White people; for people from Bangladeshi backgrounds, the odds are 1.64 times higher, and for the Black Caribbean group the chances of reporting poor health are 1.5 times higher than for White British people.
Researchers warn that these health inequalities have persisted unchanged for almost 25 years. Experts at the Centre for Aging Better are calling for government to put in place a national race equality strategy that addresses inequalities among older people and those approaching later life, including closing the ethnicity data gap.
As the new Office for Health Improvement and Disparities launches, Aging Better say government needs a clear plan for how ethnic minority older people will be supported to recover from the events of the pandemic, as this group have been disproportionately impacted by its effects. A new race equality strategy, they say, should also set out how ethnic inequalities will be tackled across the life course, to prevent them widening in later life. In addition, government should assess the potential impact on different ethnic groups of the upcoming review of the State Pension age.
Dr. Laia Becares, Senior Lecturer in Applied Social Science at the University of Sussex, said: "We find that ethnic inequalities in later life are persistent. Racism is a well-documented driver of ethnic health inequalities, and its accumulation over people's life is associated with the stark health inequalities we see.
"Racism impacts on health directly, through higher blood pressure and stress for example, but it also has indirect effects through social inequalities that reduce people's life chances, by leading to poorer housing standards, lower pay, reduced employment opportunities, and other factors that damage health over people's lives.
"Our research pools together all available data existent to study ethnic inequalities in health in later life in the UK. But there is a dearth of data to study ethnic minority older people, and so there is much more that can still be learnt about the lifecourse process that leads to ethnic inequalities in aging."
Aideen Young, Senior Evidence Manager at the Centre for Aging Better, said: "This study reveals really shocking health inequalities between different ethnic groups, with some groups experiencing the rates of poor health that White people typically see at much older ages.
"It's also depressing to see that these inequalities haven't changed for the last 25 years. In the wake of the pandemic, we risk seeing them widen—so it's vital that government makes tackling health inequality a priority in the recovery.
"To properly address the problem we need much better data, which is why we are calling for ethnicity data reporting to be mandatory for all official data monitoring. We also need to see a national race equality strategy put in place. And government must do more to address inequalities among those in and approaching later life where, as we can see from these figures, those inequalities often widen."
More information: Sarah Stopforth et al, Ethnic inequalities in health in later life, 1993–2017: the persistence of health disadvantage over more than two decades, Ageing and Society (2021). DOI: 10.1017/S0144686X2100146X