Study finds that patients with alcohol-associated cirrhosis have worse outcomes in recovering from critical illness

Patients with alcohol-associated cirrhosis have poorer outcomes after ICU discharge, compared to patients with cirrhosis linked to other causes, according to new Mayo Clinic research.
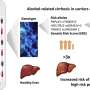
Cirrhosis is a scarring of the liver that damages function and can be life-threatening. Almost half of all cirrhosis deaths are attributed to chronic alcohol use disorder, with the rest caused by hepatitis and other forms of liver disease. Over 7 deaths per 100,000 worldwide are linked to alcohol-associated cirrhosis.
According to the new study published in Mayo Clinic Proceedings, patients with alcohol-associated cirrhosis had significantly higher post-ICU, in-hospital death rate ― 10% versus 6.5% ― as well as higher mortality at the 30-day benchmark after ICU discharge ― 18.7% versus 11.2% ― than patients with cirrhosis attributed to other causes.
"Clinical outcomes of patients with alcohol-associated cirrhosis have been reported in previous studies, with conflicting results," says Douglas Simonetto, M.D., a Mayo Clinic gastroenterologist and the study's senior author. "Our study demonstrates that although there is no significant difference in ICU mortality in patients with ALC, as compared to other causes, there was a significant difference in mortality for patients who survive their ICU stay up to 30 days later."
Previous studies have attributed a higher prevalence of infection as the reason for increased mortality in patients with alcohol-associated cirrhosis, compared to patients without alcohol-associated cirrhosis. "In our study, the infection rates were similar among the two groups," Dr. Simonetto says. "But when infection was present, it was associated with higher mortality in ALC."
The retrospective study analyzed case files for 1,174 patients who were admitted to the ICU at Mayo Clinic between January 2006 and December 2015. Patients were about evenly split between those with alcohol-associated cirrhosis and those with cirrhosis linked to other causes. Researchers focused on survival rates within the ICU, after the ICU and in the hospital, and at 30 days after being discharged from the ICU.
The mean age of patients in the study was 59, and 60% were male. Among alcohol-associated cirrhosis patients, 69.2% had cirrhosis caused by alcohol use alone and 30.8% had cirrhosis due to alcohol plus an additional cause, such as viral hepatitis C. About half of the patients with alcohol-associated cirrhosis continued to drink until the ICU admission, while 36.7% quit six months or longer before admission.
"Surprisingly, there was no significant difference in survival for patients who abstained from alcohol six months or more before ICU admission and those who did not," says Chansong Choi, M.D., a Mayo Clinic internal medicine resident and the study's lead author. "This may reflect too short a period of abstinence, as other studies have suggested that at least one to 1½ years of abstinence might be needed to make a significant difference in survival outcomes in patients with ALC."
Early diagnosis of sepsis, a potentially life-threatening condition that occurs when the body's response to infection damages its own tissues, is critical in patients with cirrhosis who are admitted to the ICU. Quick Sequential (Sepsis-Related) Organ Failure Assessment (qSOFA) has been proposed as a simple tool for early detection of sepsis, but the Mayo Clinic study finds qSOFA has limited clinical usefulness and applicability for patients with cirrhosis.
"Our study finds that qSOFA is a poor prognosticator of sepsis and in-hospital mortality among patients with cirrhosis," says Dr. Choi. "We need better bedside tools to predict infection and sepsis in these patient groups so we can implement the appropriate therapeutic measures."
The authors report no competing interests or financial disclosures.
More information: Relationship Between Etiology of Cirrhosis and Survival Among Patients Hospitalized in Intensive Care Units, Mayo Clinic Proceedings (2022). DOI: 10.1016/j.mayocp.2021.08.025 , secure.jbs.elsevierhealth.com/pb-assets/Health%20Advance/journals/jmcp/jmcp_ft97_1_3.pdf