Study: Prevention suffers when doctors drop out of Medicare's ACO program
For 10 years, the agency that runs Medicare has offered doctors and their practices extra money if they joined groups called Accountable Care Organizations and improved the quality of care they provided to older patients covered by traditional Medicare, while also focusing on the cost of their care.
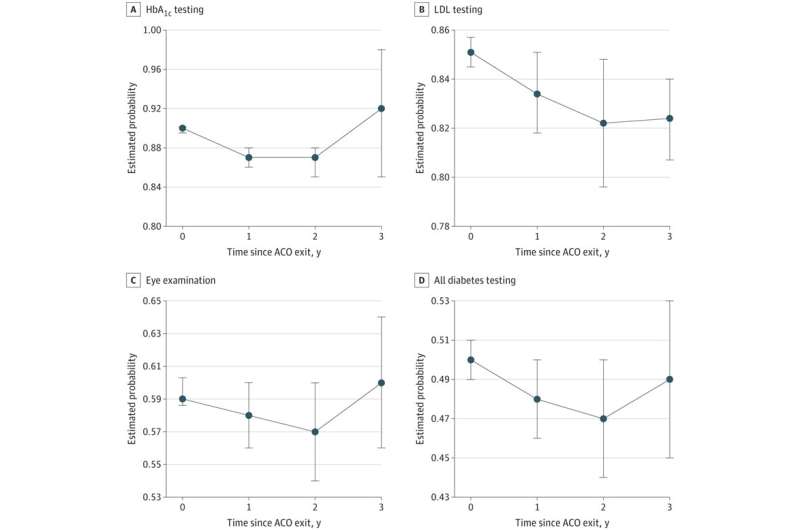
But a new study finds that those quality gains erode quickly when physician groups leave ACOs—which many have done in the past two years. After they dropped out, their patients with diabetes were less likely to get important preventive services, such as screening for high blood sugar or high cholesterol, and eye exams to check for the damage their disease can do.
The new findings were published in JAMA Health Forum just before the release of new data about this year's ACO enrollment by the Centers for Medicare and Medicaid Services (CMS).
The new study's lead author, Yajuan Si, Ph.D., of the University of Michigan Institute for Social Research, notes, "While more than 11 million older Americans receive care from at least one of the 529,000 physicians or other providers who take part in any one of 483 ACOs, those numbers are down from peaks in 2020. Our findings highlight the need to monitor quality at exiting practices."
The new study, also led by John Hollingsworth, M.D., M.Sc., of the U-M Medical School, looks at data from more than 1.7 million older adults whose providers were enrolled in ACOs taking part in the Medicare Shared Savings Program through 2016.
In the first two years after their providers' practices left an ACO, older adults received fewer screenings than their counterparts whose providers stayed in an ACO. However, there was no difference in the two groups' emergency department visits or hospital admissions. Preventive care showed signs of rebounding in the third year after a group dropped out of an ACO.
"The addition of 'downside risk' to the Shared Savings Program under a recent program overhaul, which means ACOs can lose money if they don't achieve goals for improving quality of care or containing cost growth, and the cost of paying for systems and staff to drive improved care, may have contributed to the issue," Hollingsworth notes.
More information: Yajuan Si et al, Use of Preventive Care Services and Hospitalization Among Medicare Beneficiaries in Accountable Care Organizations That Exited the Shared Savings Program, JAMA Health Forum (2022). DOI: 10.1001/jamahealthforum.2021.4452



















